This Medical Charity Made $3.3 Billion From a Single Pill
How the Cystic Fibrosis Foundation amassed a fortune—and upended medical research at the same time
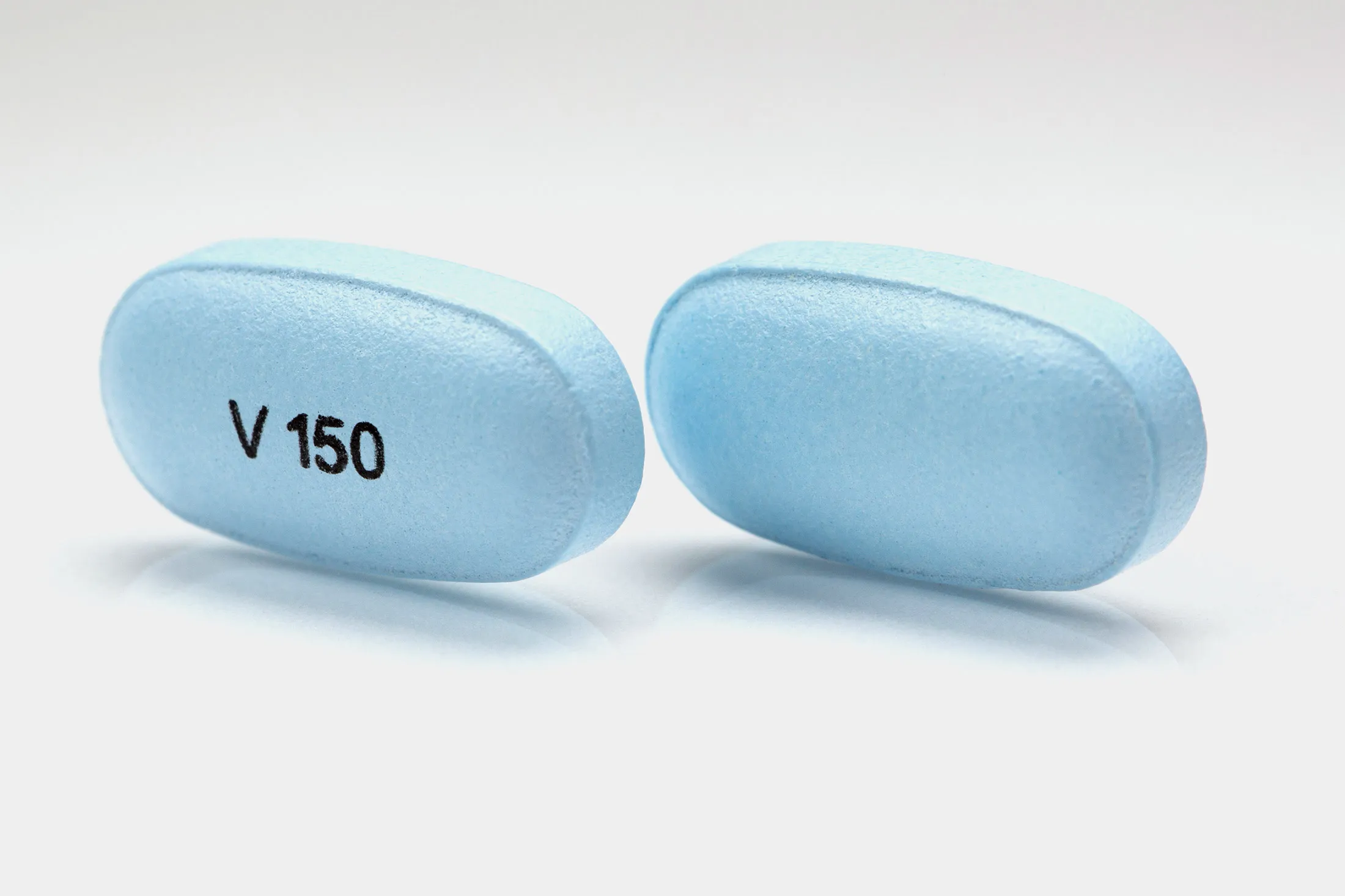
Kalydeco, approved by the FDA in 2012, can treat cystic fibrosis in about 2,000 patients in the U.S. A year's supply costs more than $300,000.
Source: Vertex Pharmaceuticals