Here’s How Affordable Care Act Marketplaces Are Shaping Up Under Trump’s Watch
Many HealthCare.gov Customers See Lowest Premiums Ever
According to detailed data released Tuesday by the Centers for Medicare and Medicaid Services, subsidized marketplace customers are paying less out of pocket than ever.
More than four in five enrollees received premium subsidies to help pay for coverage, on par with previous years. Among subsidized enrollees in the 39 states using HealthCare.gov, their average cost was $89 per month, down from over $100 in each of the past three years.
For the 17 percent of HealthCare.gov customers without financial help, premiums were stiff: on average, they’ll pay $522 per month.
This is no surprise: an October, 2017 report from the Department of Health and Human Services found that 80 percent of all HealthCare.gov enrollees would be able to find a plan for $75 or less this year. Enrollment fell most sharply in areas where customers faced higher monthly payments.
After a Chaotic Year, Marketplaces Enroll Millions
It’s been a tumultuous year for the Affordable Care Act marketplaces. The Trump administration and Congress tried and failed multiple times to repeal the Affordable Care Act, and then successfully repealed the law’s individual mandate as part of the tax reform bill President Donald Trump signed into law in December. The Trump administration slashed funding for advertisement and enrollment assistance and halted some subsidy funding, which sent insurers scrambling all summer long to determine where to offer plans for 2018, and for how much. With all these changes, enrollment was widely expected to tumble this year.
But it didn’t.
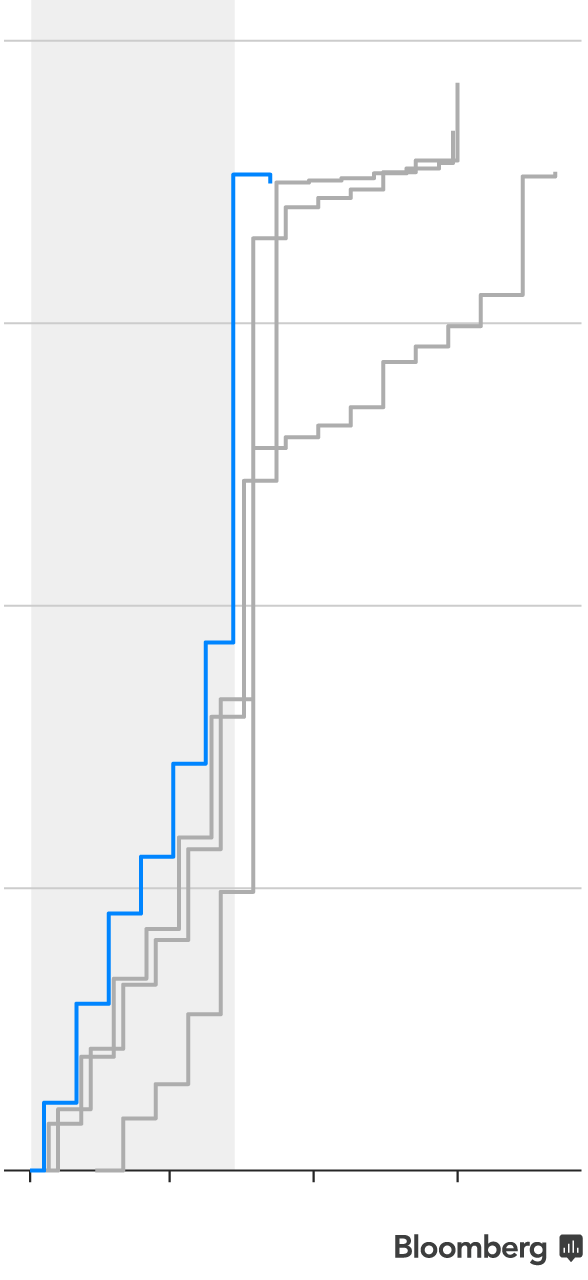
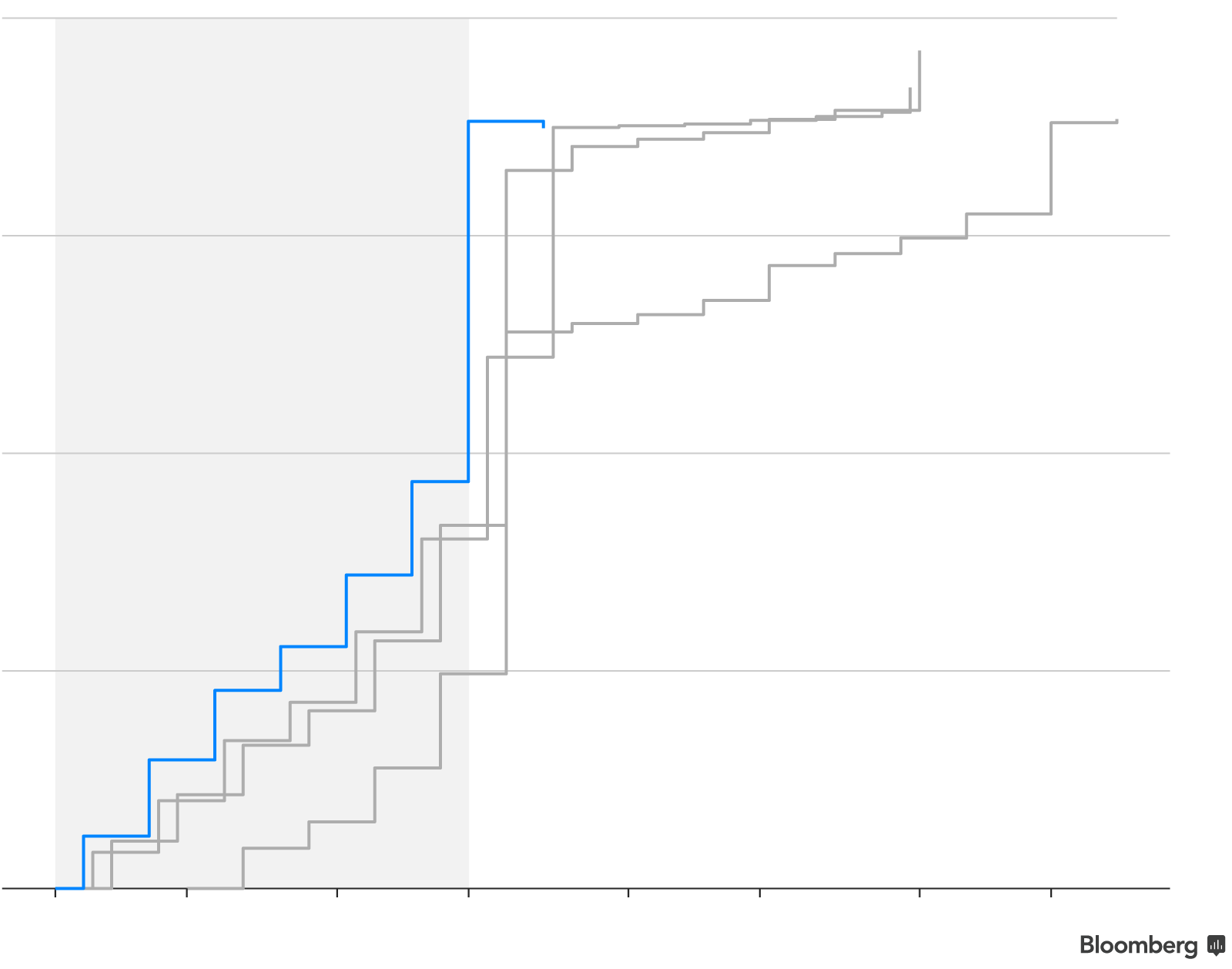
Nearly nine million people selected marketplace plans in the 39 states using HealthCare.gov during open enrollment. Even though this year’s six-week enrollment period was half the length of previous years, enrollment fell only five percent from last year.
10 million
2016
2018 open enrollment period
2017
2018
2015
7.5
5
2.5
0
Nov.
Dec.
Jan.
Feb.
10 million
2016
2018 open enrollment period
2017
2015
2018
7.5
5
2.5
0
Nov. 1
15
Dec. 1
15
Jan. 1
15
Feb. 1
15
Note: Data includes 39 states in 2018 and 2017, 38 states in 2016 and 37 states in 2015. Plan year 2018 data includes cancellations of auto-enrolled plans after the open enrollment deadline, through December 23, 2017.
One reason enrollment stayed steady is that nearly all plan selections on HealthCare.gov were made by mid-December in past open enrollment periods: 95 percent last year, up from 86 percent for plan year 2016 and 72 percent for 2015. Though December 15 wasn’t the final deadline in past years, it was the last day to sign up for plans that start January 1. In addition, existing customers who haven’t actively chosen a plan for the upcoming year are automatically reenrolled in the same plan or a similar one around the same time—2.8 million people last year.
Another reason enrollment didn’t dip dramatically: many customers could still find cheap plans.
After the Trump administration stopped making some subsidy payments, insurance companies in most states raised prices on certain plans to compensate. As a result, subsidized customers, who are generally insulated from rate increases, were able to find more deals than ever. Four out of five customers on HealthCare.gov were eligible for plans costing $75 or less per month, according to to the Trump administration’s own data, and many were eligible for plans with no premium charges.
A record number of companies exited the marketplaces this summer, but that didn’t necessarily put a damper on enrollment, either. Humana, Aetna and several Anthem subsidiaries left many markets they operated in last year, citing political uncertainty and financial losses. Based on preliminary state-level data, even states with widespread insurer exits, including Iowa and Nevada, had similar enrollment to past years. And in eight states that use HealthCare.gov and eight state-based marketplaces, enrollment increased over last year.
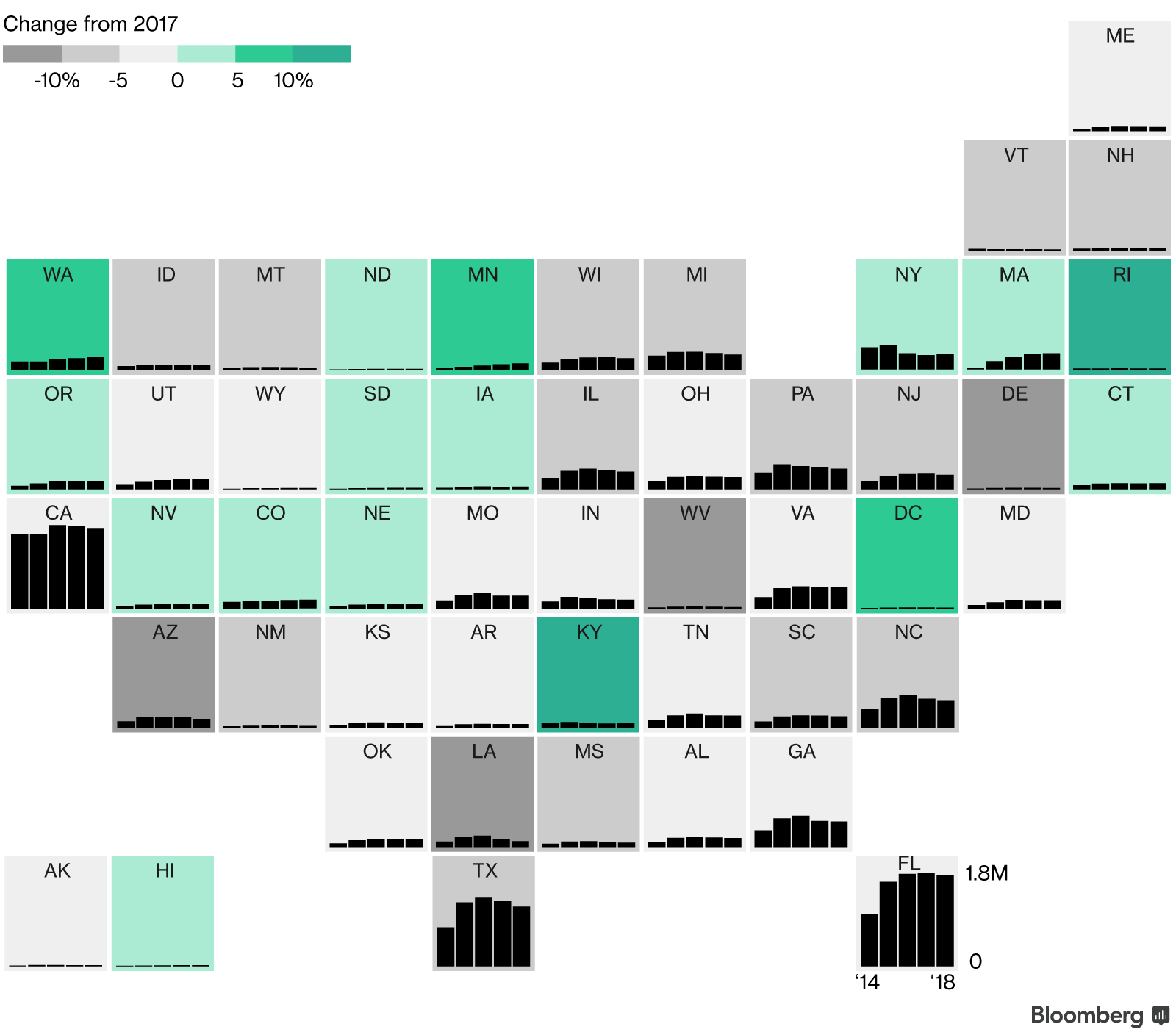
In spite of the shortened enrollment period, regulatory changes and legislative threats, dire predictions about the 2018 marketplaces failed to materialize. Though President Trump claims that he has “essentially repealed Obamacare,” every county has at least one company selling plans, and millions of new and returning customers again purchased insurance that covers the ACA’s essential health benefits.
But without major administrative changes, the marketplaces are on track for more of the same in 2018: more company exits and rising prices, accompanied by increased subsidies to cover those costs for those who qualify.
Missed the HealthCare.gov Deadline? You May Still Be Able to Enroll
Open enrollment for 2018 marketplace plans in 41 states ends in the early-morning hours on Saturday. But some people will get more time to sign up.
As happens every year, hoards of last-minute shoppers jam the phone lines trying to enroll. The government will give them a couple of extra days to finish their application as long as they tried to sign up before the deadline.
And millions more will get even more time to sign up.
For starters, anyone that lives in the District of Columbia and nine states that operate their own marketplaces has more time to apply. These states, where nearly 3 million people enrolled last year, set their own deadlines, which range from Dec. 22 to Jan. 31.
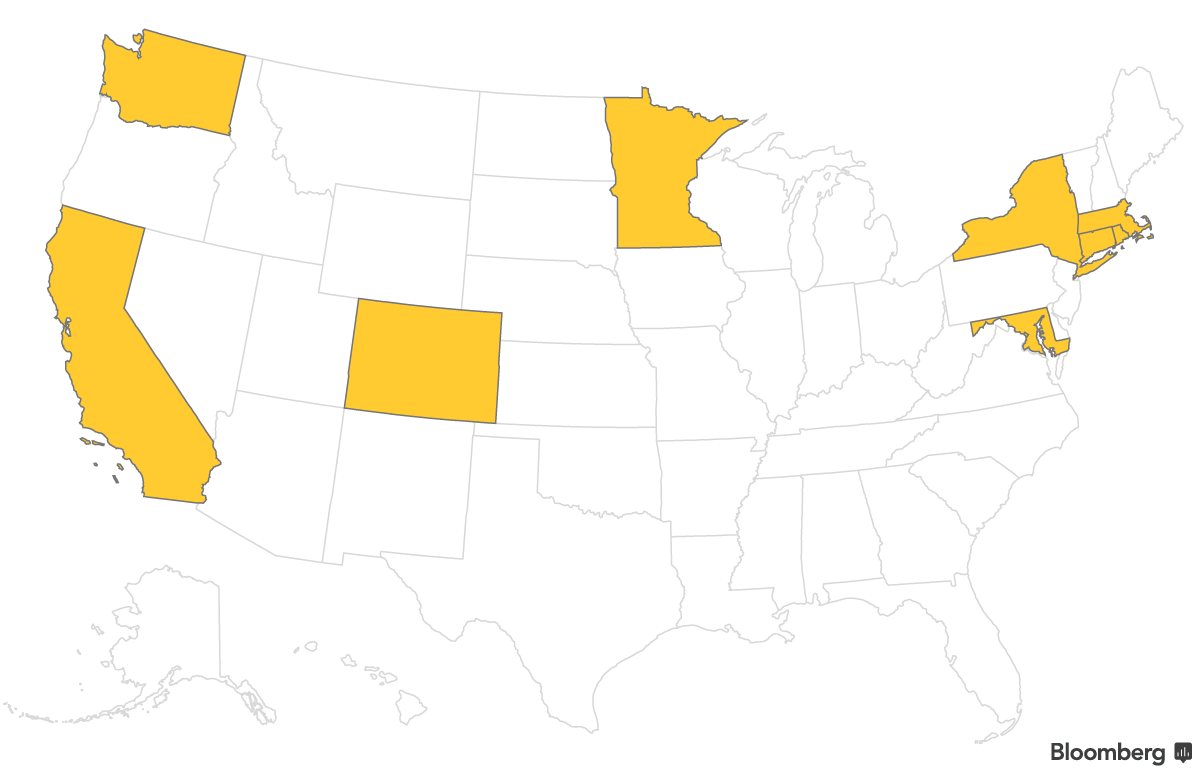
Residents of areas affected by Hurricanes Irma, Harvey and Maria qualify for a special enrollment period running through Dec. 31.
On December 19 CMS confirmed that individuals living in counties that are receiving FEMA assistance for other hurricanes or hurricane-related events, including Hurricane Nate, would also be eligible for the extended enrollment period.
People who live in Alabama, Florida, Georgia and South Carolina, as well as some parts of Louisiana, Mississippi and Texas qualify for this hurricane-related extra time. Last year, 3.5 million people in these areas enrolled in plans. Though Puerto Rico does not have a health insurance marketplace, Puerto Ricans who have moved to the mainland since Hurricane Maria may also qualify for this special enrollment period.
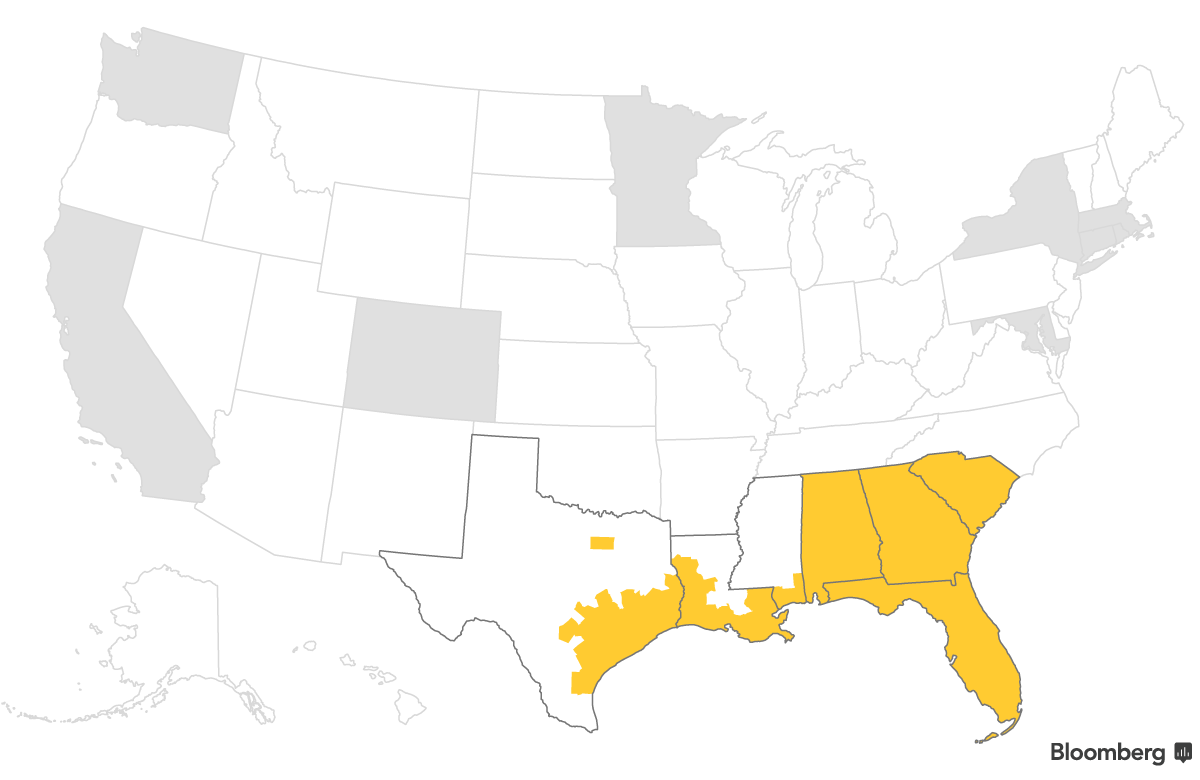
If your insurer in 2017 is not offering plans in your county next year, or significantly changing your plan, you get more time, too. Though HealthCare.gov and state marketplaces will automatically assign nearly everyone who lost their insurer to similar plans from other insurance companies, federal rules give those people until March 1, 2018 to choose a different plan if they haven’t yet.
There are 120 counties where every insurance company that sold marketplace plans in 2017 is exiting. About 153,000 people enrolled in those counties last year and can take advantage of the extended deadline if they haven’t yet chosen a plan with a new company.
At least one insurer exited about half of all U.S. counties this year, where more than five million current enrollees live. Based on available data, hundreds of thousands of people will likely qualify for more time.
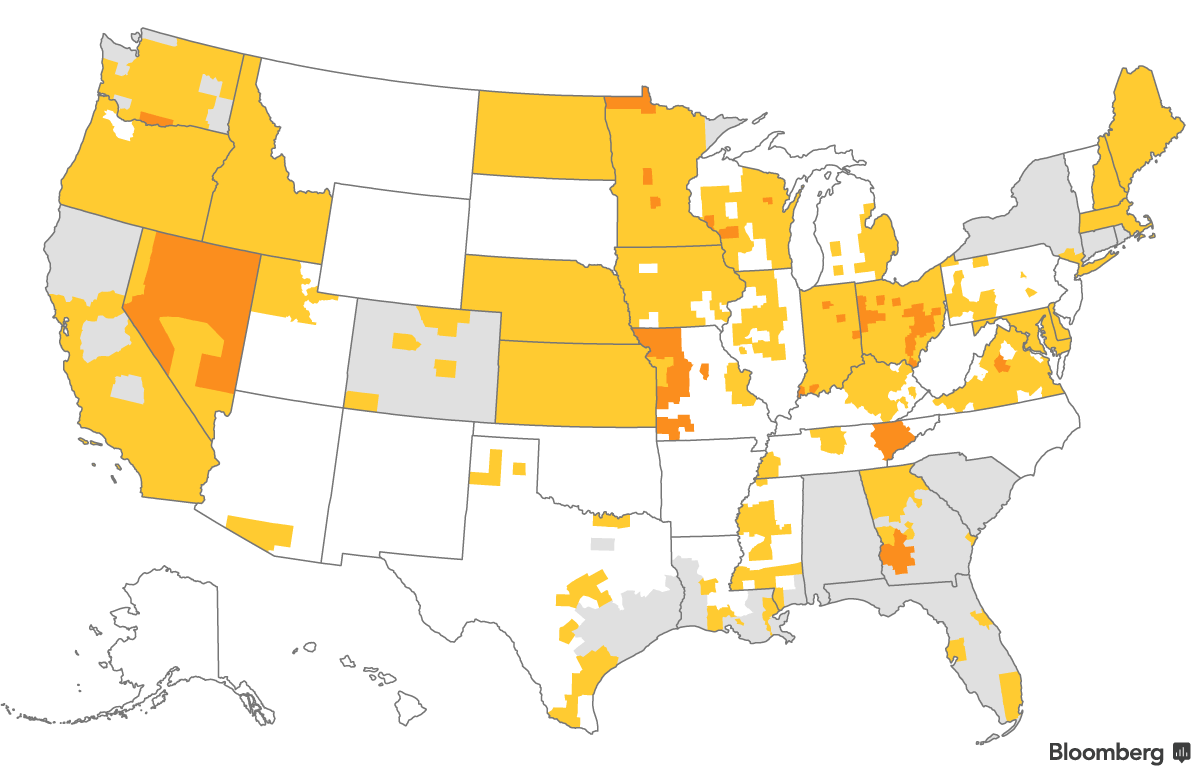
In total, some customers in more than half the country will have more time to select health insurance plans for next year.
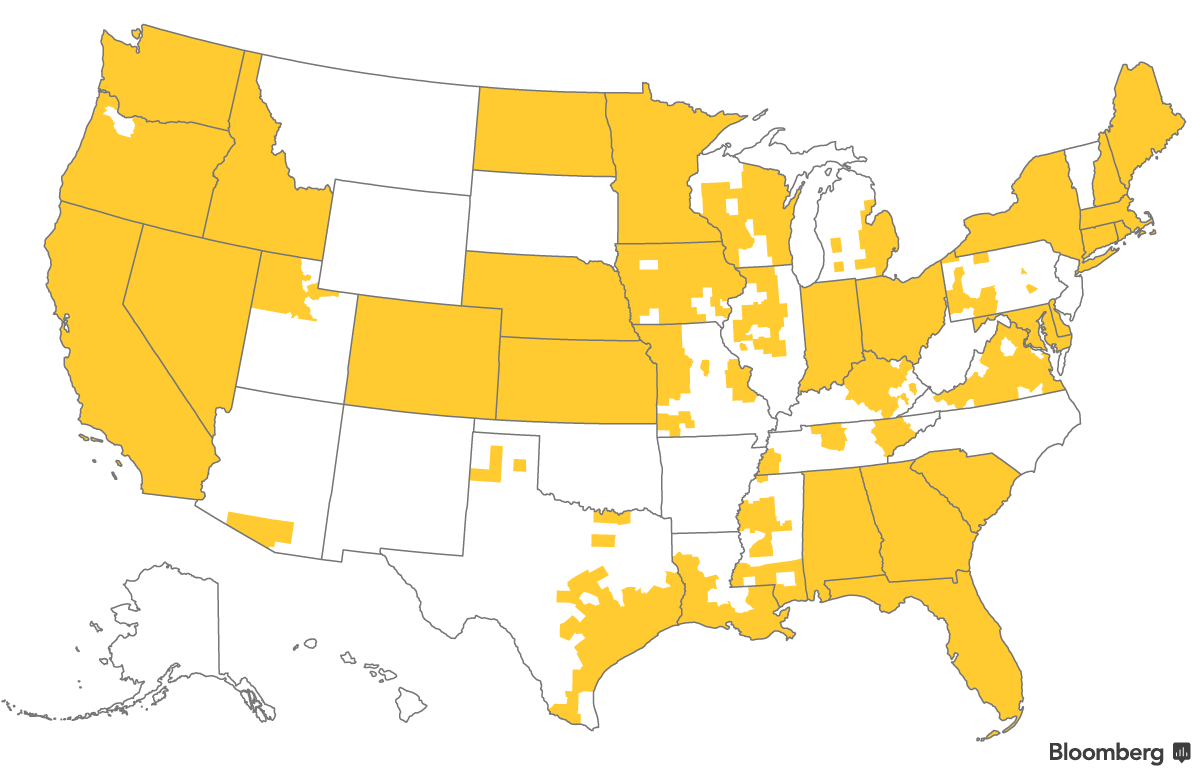
We should know more about people who signed up soon. Preliminary open enrollment data from HealthCare.gov—excluding special enrollment periods—are expected next week.
Thousands Select Free Health Plans in Marketplace Quirk
As open enrollment draws to a close in most states, a surprising trend is emerging: Thousands of people are finding, and choosing, free plans for 2018.
Midwestern insurer Medica announced today that 24,000 of their customers have chosen plans with no monthly premiums after subsidies for 2018. Most live in Iowa and Nebraska, where Medica is the only marketplace insurer. About 17,000 Nebraskans, half of the state’s enrollees as of late November, have chosen no-cost plans. Another 5,000 have chosen no-cost plans in Iowa.
These free plans can still come at a price. Most are bronze-tier plans, which have average deductibles of about $6,000 and high copays.
According to the Department of Health and Human Services, 80 percent of HealthCare.gov enrollees will be able to find a plan with monthly premiums of $75 or less in 2018, up from previous years. But the free plans that so many Medica customers are choosing were not as widely available in the past. Whether the prevalence of these free plans is widespread will be clearer after open enrollment ends on Friday in 42 states.
2018 Marketplace Participation
It’s been a rocky year for the Affordable Care Act amid regulatory rollbacks and several failed attempts to repeal the law. But insurers have largely navigated the uncertainty and finalized their marketplace plans for 2018. Bloomberg News analyzed insurance filings and spoke with companies and state agencies all summer to make sense of how the marketplaces took shape ahead of open enrollment, which begins Nov. 1.
Based on the latest data, nearly half of the 12 million people who got health insurance through Obamacare’s individual marketplaces will have the same number of companies to choose among next year as they did in 2017, while 10 percent will have more options. Forty-two percent will have fewer companies to choose among.

Most marketplace enrollees had multiple insurance companies to choose among this year, and most will again in 2018. In 2017, 83 percent of enrollees received help paying their premiums.

Correction: A previous version of this graphic excluded data for renewing California enrollees in 2017. The total number of enrollees for California counties have been updated to reflect the change.
Previous Updates
You May Not Need to Switch Insurers to Find a Better Plan
This year, price-conscious marketplace customers can typically find good deals for less. But for many customers, price isn’t the only thing driving their decision. Higher-priced insurers often have larger networks of doctors and hospitals than low-cost companies, and changing insurers for a cheaper plan can be more of a hassle than it’s worth.
Those customers may find good deals, too.
Here’s an example: Let’s say you’re a 40-year-old with a chronic medical condition who earns $42,000 per year in Orange County, California. At that income, you’ll qualify for a $66 per month premium subsidy for 2018. Since you know you’ll need to visit the doctor regularly and buy monthly prescriptions, you’re not interested in high-deductible bronze plans.
You bought a silver plan in 2017 through Kaiser Permanente. Slightly cheaper plans are available this year from Blue Shield, Centene’s Health Net or Oscar Health Plan, but that might require that you switch doctors. Alternatively, you can stick with Kaiser Permanente and switch to a no-deductible gold plan for $17 less than their silver plan on California’s marketplace.
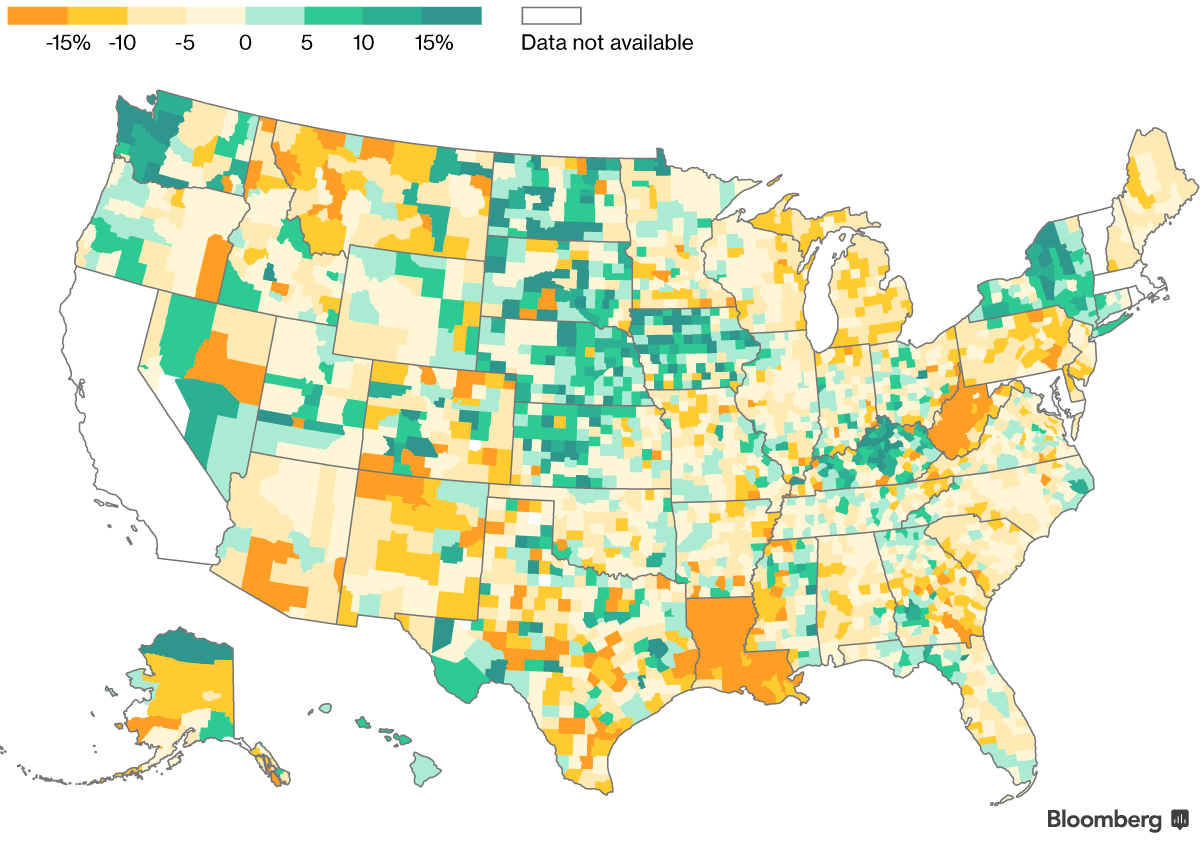
Under the Affordable Care Act, gold plans are designed to cover about 80 percent of medical expenses. Silver plans cover 70 percent and bronze plans 60 percent. In past years, that meant gold plans cost more than silver, which cost more than bronze. But this year, thanks to a weird consequence of President Donald Trump's decision to cut off some insurer funding, that isn't always the case.
In 16 states, at least one company is selling their cheapest gold plan for less than their cheapest mid-level silver. And in other places, those superior gold plans are only a few dollars more. They might not be the cheapest option available, but for customers intent on sticking with the same insurer, gold deals abound.

Note: Monthly premiums are shown by county for a 40-year-old individual without premium subsidies. Data was not yet available for Massachusetts and New York. The map shows the minimum difference in each county between each company’s cheapest gold plan and cheapest silver plan.
Trump Order to End Subsidy Payments Shakes ACA Marketplaces
President Donald Trump's decision to halt payments on subsidies for low-income enrollees is likely to send ripples through the market. Under the Affordable Care Act, marketplace insurance companies are required to lower deductibles and prices for doctor’s visits and other services for many enrollees. Until now, the federal government has picked up the tab, reimbursing insurers about $7 billion this year alone.
In 2017, 58 percent of all marketplace enrollees received cost-sharing reductions (CSRs)—in some areas, almost all enrollees did. Insurers are still required to reduce costs for these roughly seven million enrollees. Without the reimbursement, insurers will have little choice but to hike rates or decide to not offer plans at all.

Note: State-level data is shown for states that do not use HealthCare.gov.
This isn't a surprise to insurers, which had already assumed that the Trump administration would end CSR payments and raised prices accordingly to cover predicted losses in states that allowed it. Some state insurance departments requested two sets of rates depending on the fate of the subsidies, while others required insurers to assume that CSRs would continue to be paid. Medica Health Plans recently exited North Dakota after state insurance officials there would not accept Medica’s high-rate, no-CSR request.
Though insurers have already signed contracts with the federal government for 2018, the end of CSR payments gives them a potential exit clause. With less than three weeks until open enrollment, we’ll be watching closely to see if other companies choose to leave.
Some states are planning to fight back. Attorneys general from 17 states and the District of Columbia filed this summer to intervene in court if the payments were ended.
Not Repealed, Not Replaced: What’s Next for Obamacare Enrollment?
Despite a summer filled with heated repeal attempts, the Affordable Care Act’s marketplaces will open as planned on Nov. 1. As in past years, most enrollees will have multiple companies to choose among.
But that doesn’t mean it was a typical summer for state insurance departments, companies and customers waiting to see their options. Before companies signed final contracts, they entered and exited counties across the U.S.—occasionally leaving some counties with the prospect of having no insurers. In the end, all those potential bare counties were filled. Here’s how the 2018 map changed as companies waffled about whether to expand, remain or exit.
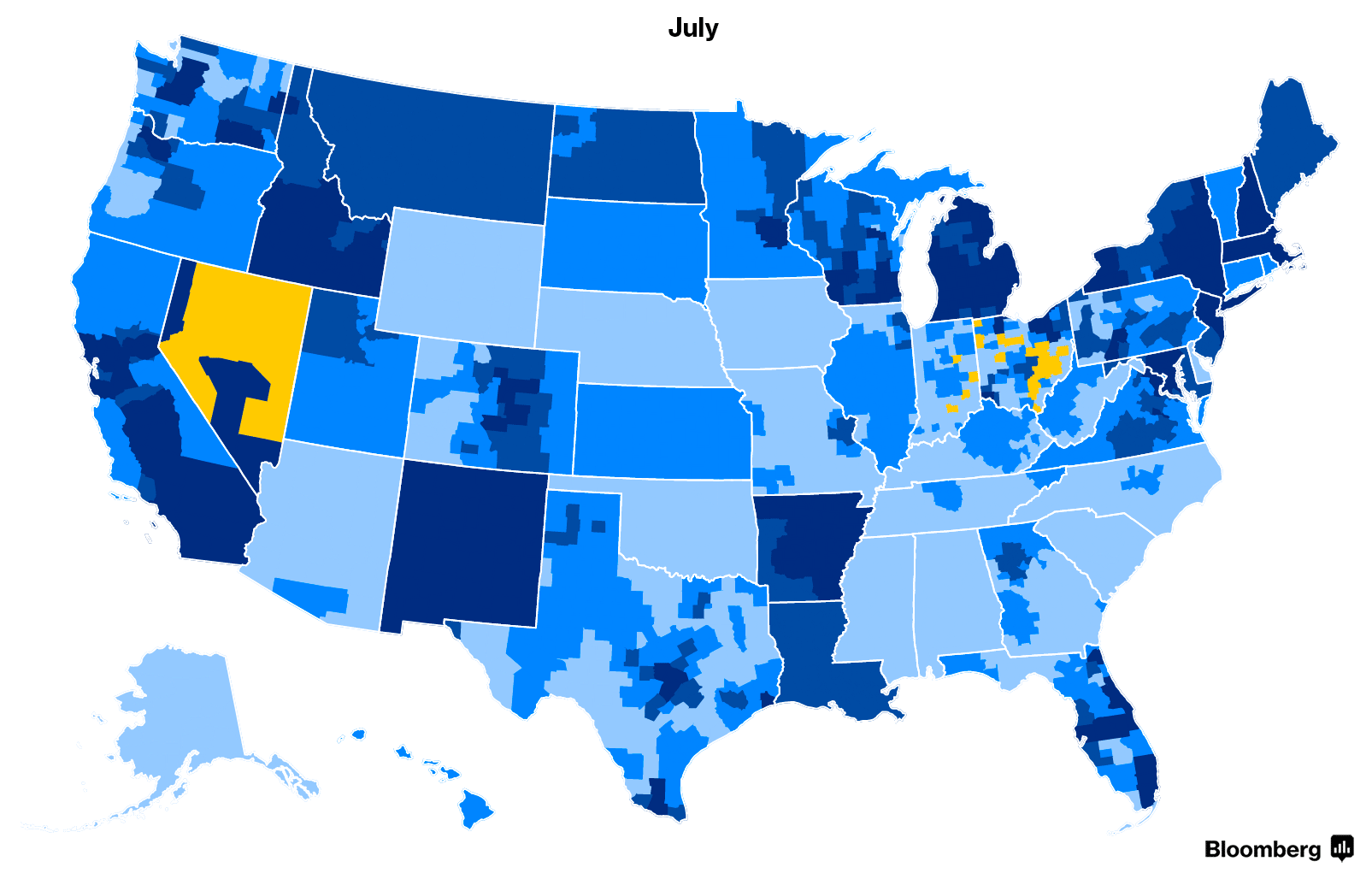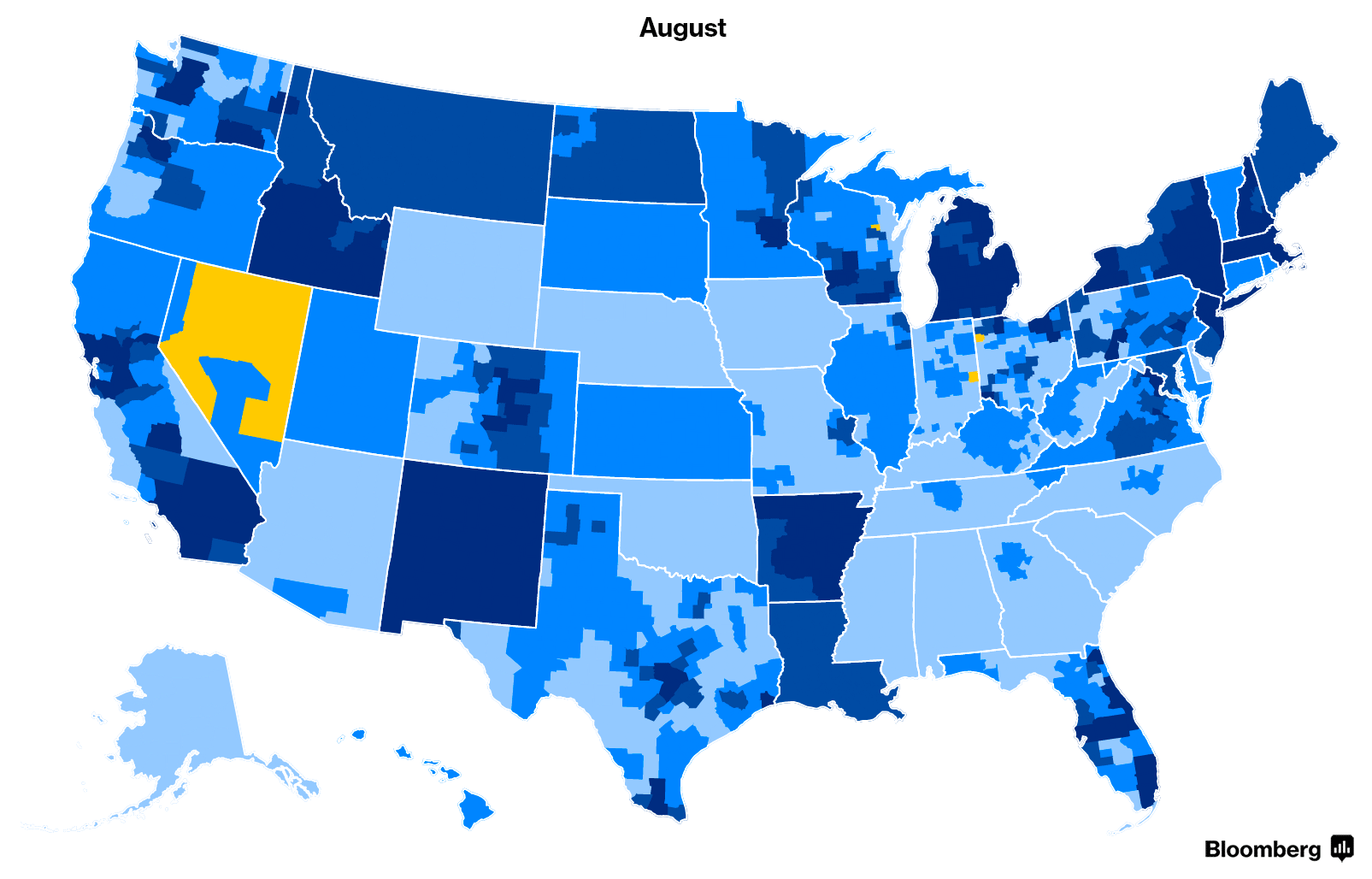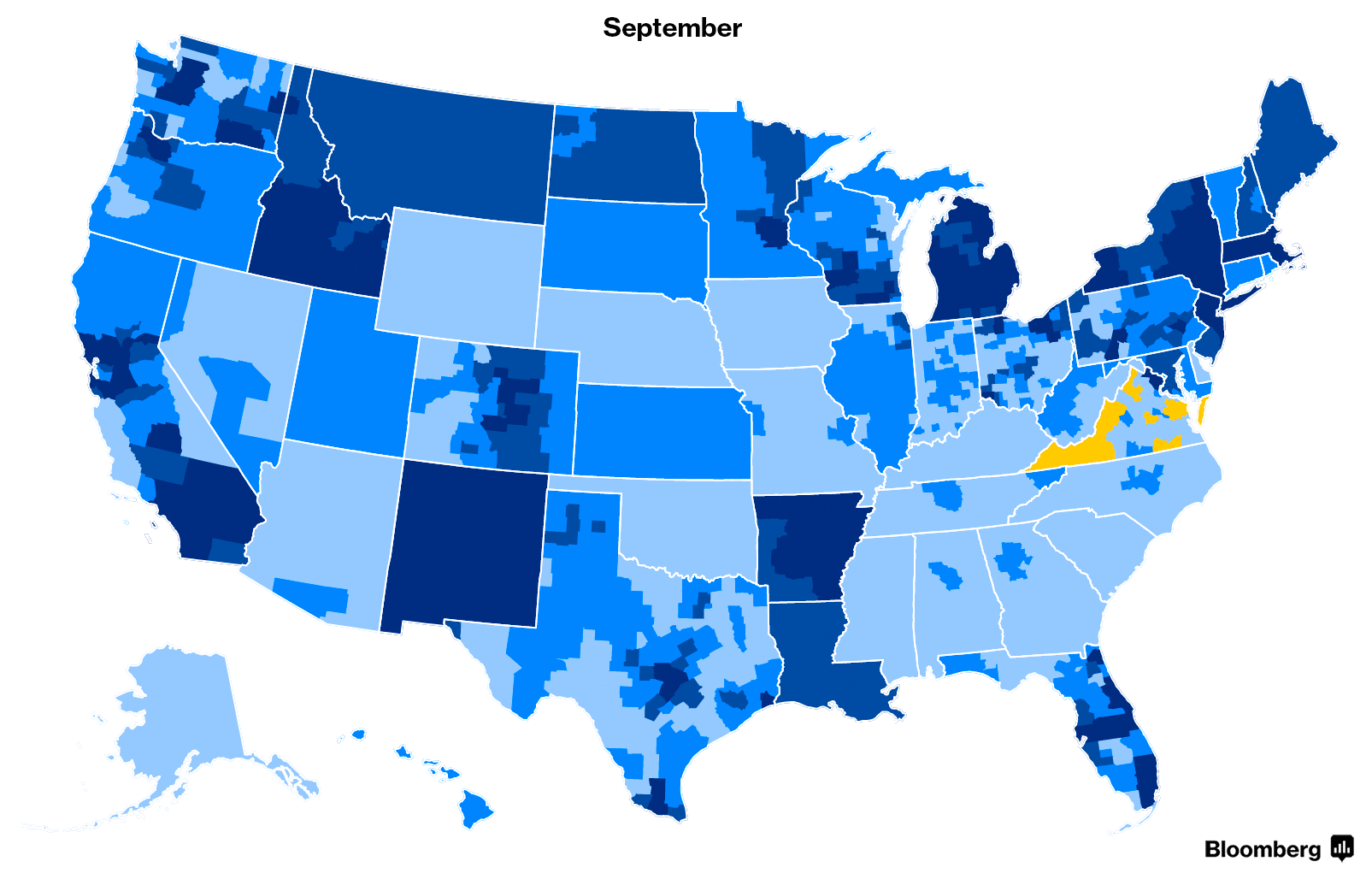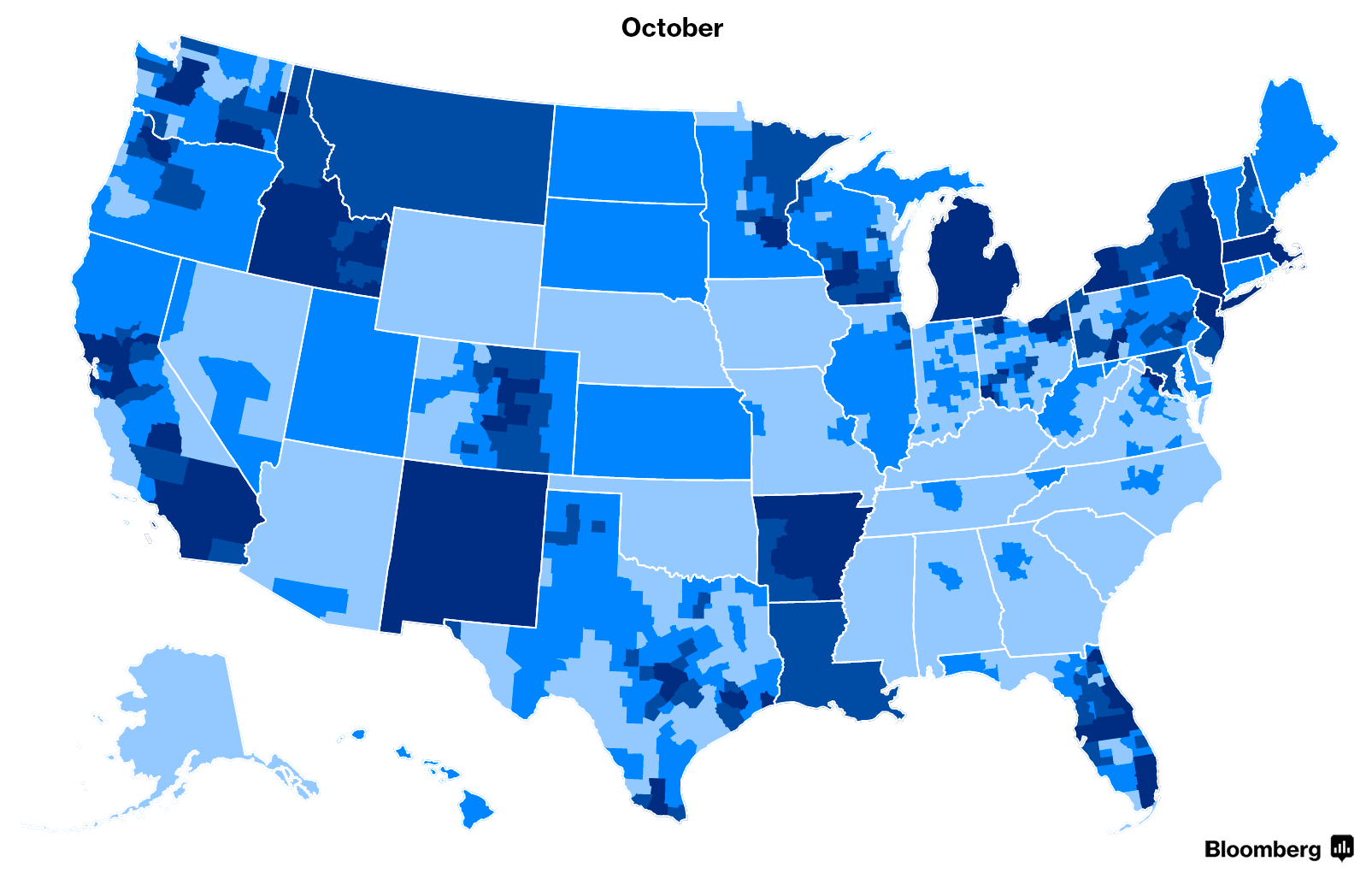
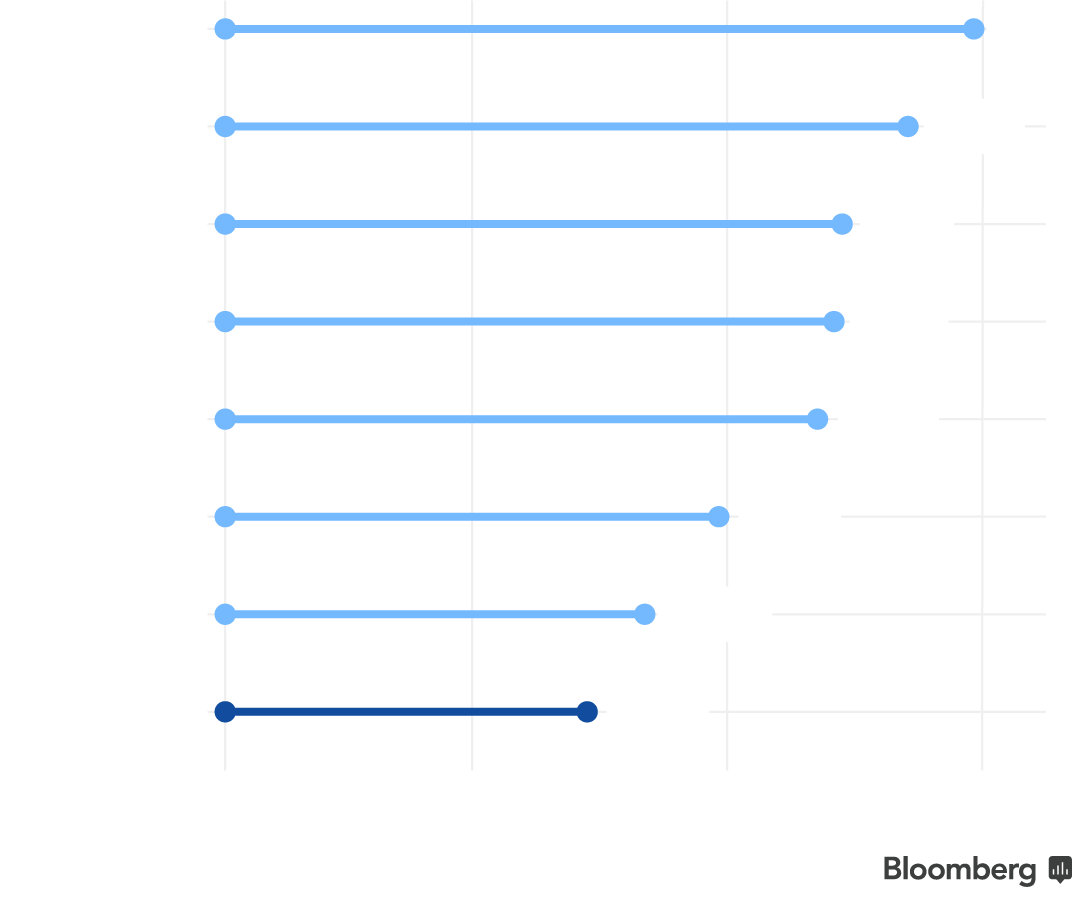
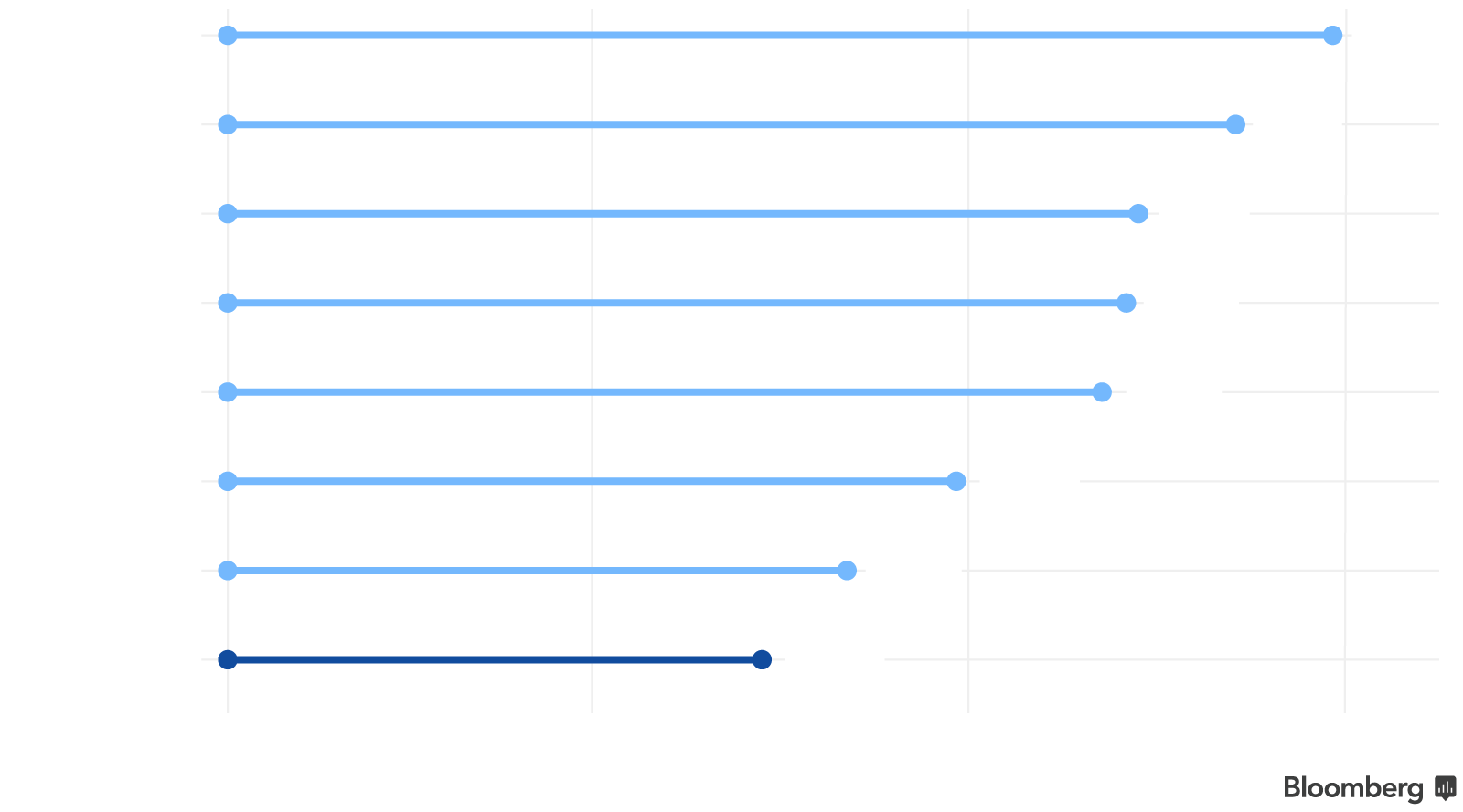
Shortened Enrollment Period
The 2015, 2016 and 2017 open enrollment periods were each three months long. This year, the standard enrollment period will run from Nov. 1 to Dec. 15, the Centers for Medicare and Medicaid Services announced in April.
Customers in 42 states will have just six weeks to shop, while most states that run their own marketplaces chose to extend their open enrollment periods.

California, D.C., New York
Jan. 31
Massachusetts
Jan. 22
Washington
Jan. 15
Minnesota
Jan. 14
Colorado
Jan. 12
Rhode Island
Dec. 31
Connecticut
Dec. 22
All 42 other states
Dec. 15
Nov. 1
2017
Jan. 1
2018
Dec. 1
Feb. 1
California, D.C., New York
Jan. 31
Massachusetts
Jan. 22
Washington
Jan. 15
Minnesota
Jan. 14
Colorado
Jan. 12
Rhode Island
Dec. 31
Connecticut
Dec. 22
All 42 other states
Dec. 15
Nov. 1, 2017
Dec. 1
Feb. 1
Jan. 1, 2018
California, D.C., New York
Jan. 31
Massachusetts
Jan. 22
Washington
Jan. 15
Minnesota
Jan. 14
Colorado
Jan. 12
Rhode Island
Dec. 31
Connecticut
Dec. 22
All 42 other states
Dec. 15
Nov. 1, 2017
Dec. 1
Jan. 1, 2018
Feb. 1
Individuals in counties affected by recent hurricanes will also have an additional two-week special enrollment period available through HealthCare.gov’s call center.
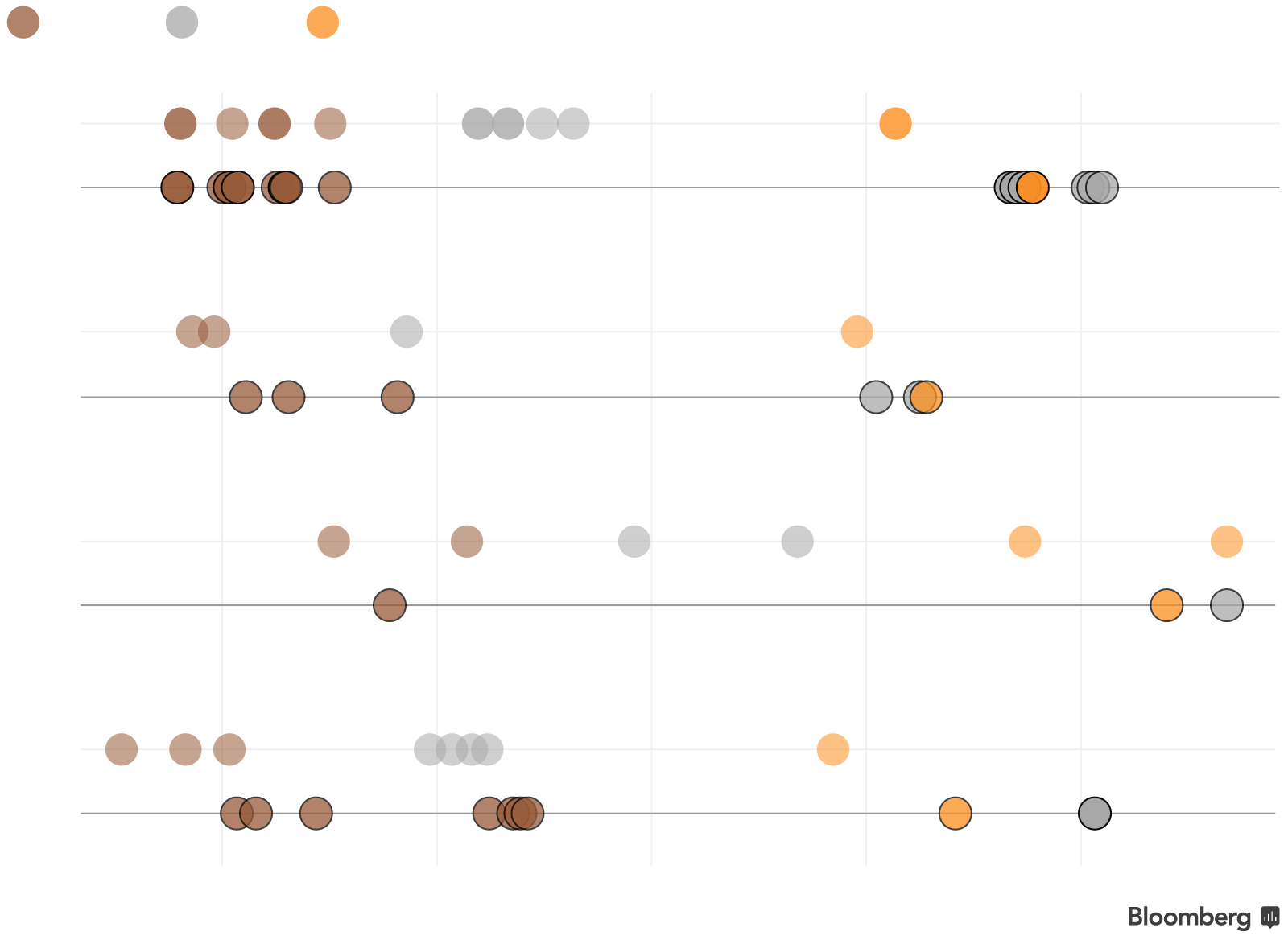
Metal Madness
The Trump administration has repeatedly threatened to not refund insurers for cost-sharing reductions (CSRs), subsidies that lower out-of-pocket costs for about seven million low-income enrollees. So far the administration has continued to make these payments, but the uncertainty has shaken insurers.
Many companies have raised rates or exited the marketplace entirely in response, while others have carefully priced certain plans to stem their losses in case CSR payments end.
Marketplace plans are generally available in four tiers, increasing in premiums and in the generosity of the benefits that they provide: bronze, silver, gold and platinum. Silver plans typically have lower monthly premiums than gold plans but have higher deductibles and higher costs to see a doctor or get a prescription drug.
Since CSRs are only available on silver plans for most people, some companies chose to drastically increase rates on those plans while keeping others relatively constant.
As a result of this targeted pricing, customers in some areas will face a new phenomenon: insurers offering gold plans at a lower price than mid-level silver plans.
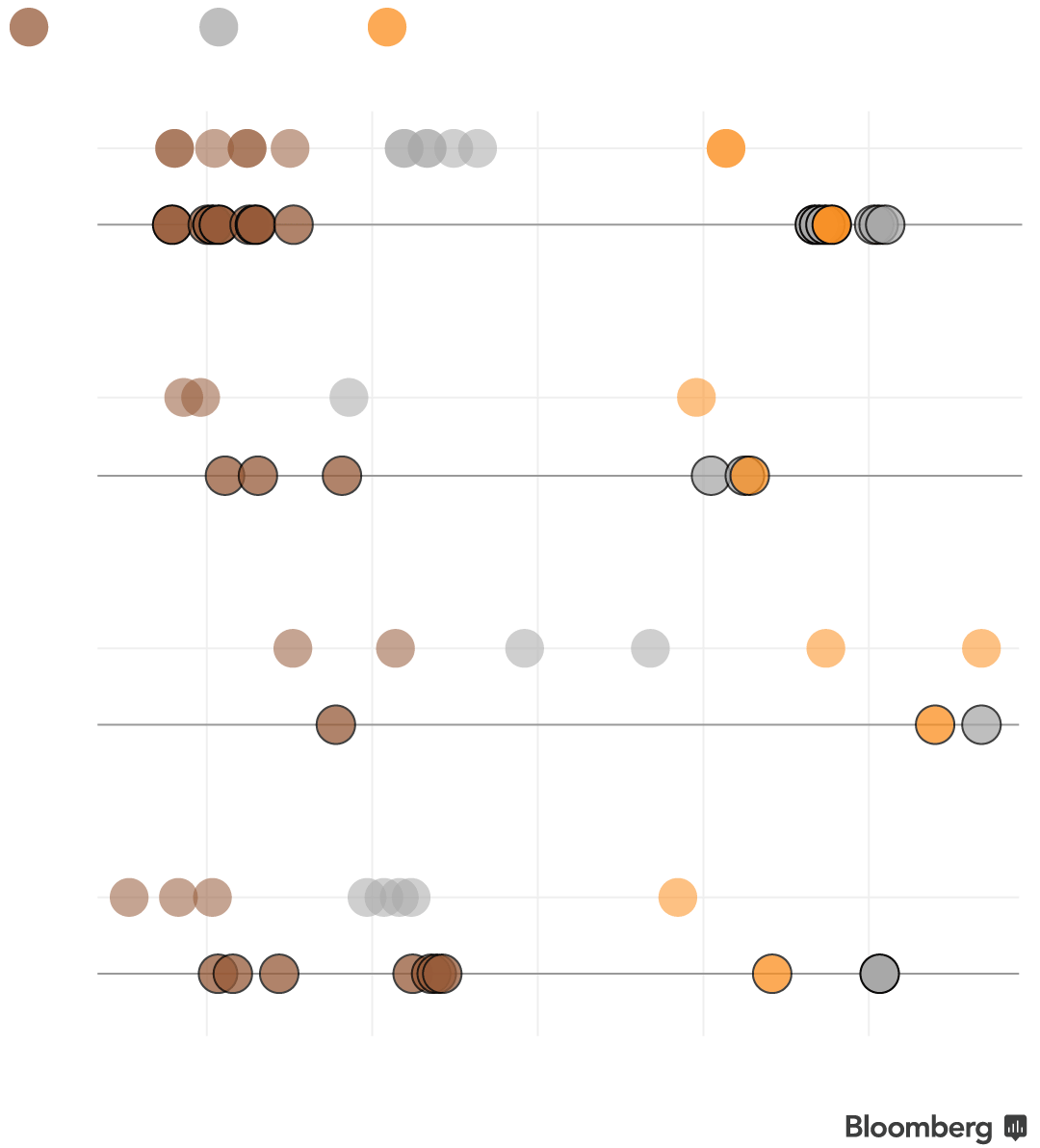
Boise, Idaho is just one place where this swap will happen. In past years, silver plan premiums were evenly spaced between bronze and gold. Silver plans for 2018 from all four Idaho insurers will be either similarly priced or more expensive than the companies’ more generous gold plans.
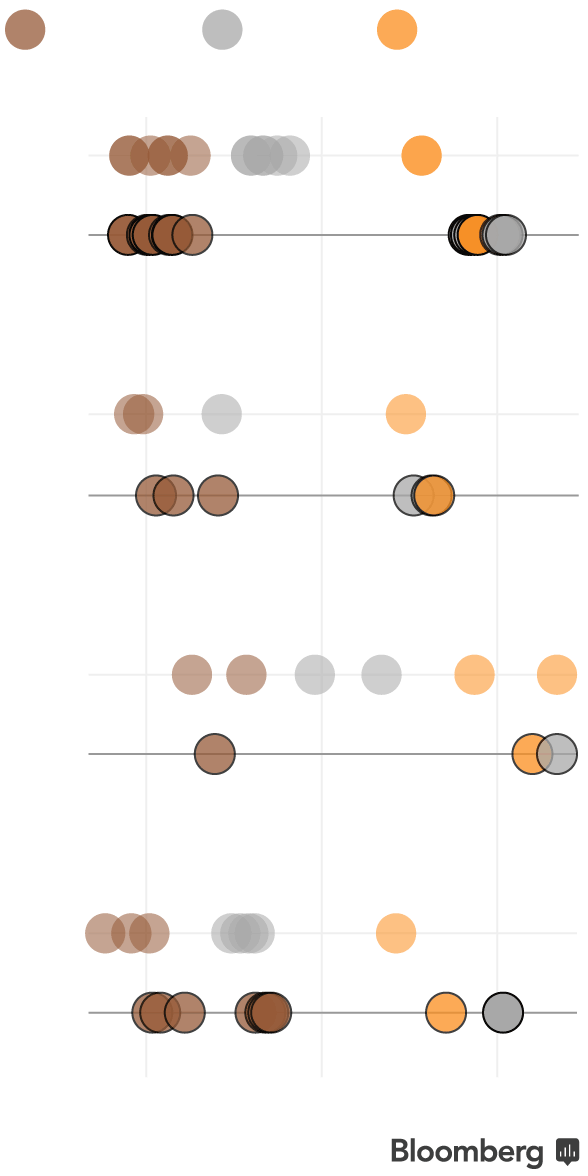
Bronze
Silver
Gold
Blue Cross of Idaho
2017
2018
Mountain Health CO-OP
2017
2018
PacificSource Health Plans
2017
2018
SelectHealth
2017
2018
$300 monthly premium
$400
$500
Bronze
Silver
Gold
Blue Cross of Idaho
2017
2018
Mountain Health CO-OP
2017
2018
PacificSource Health Plans
2017
2018
SelectHealth
2017
2018
$350
$400
$450
$500
$300 monthly premium
Bronze
Silver
Gold
Blue Cross of Idaho
2017
2018
Mountain Health CO-OP
2017
2018
PacificSource Health Plans
2017
2018
SelectHealth
2017
2018
$300 monthly premium
$350
$400
$450
$500
Note: Premiums shown are for a 40-year-old in Ada County, Idaho without premium subsidies. BridgeSpan, which sold marketplace plans in 2017 but will not in 2018, is not shown.
Subsidized customers may not see a difference in the amount they’re expected to pay next year since federal assistance increases with the cost of silver premiums. This year, 71 percent of enrollees chose silver plans. But enrollees in some states, including Idaho, will find that switching to a gold plan will offer more for less money.
We’ll see if customers choose to switch plans. In past years, customers only tended to switch plans if their costs after subsidies had significantly increased. Nearly 2.8 million enrollees in 2017 chose not to shop for a new plan and were automatically re-enrolled into the same plan or a similar one.
Anthem Exits Maine on Filing Deadline Day
On Wednesday, the deadline in most states for insurers to finalize their 2018 Affordable Care Act plans, Anthem announced that it will exit the marketplace in Maine. Due to a state law, Anthem’s current Maine enrollees may renew their plans for 2018 outside of the marketplace but will no longer be eligible for financial assistance. Maine enrollees will have two marketplace companies to choose among next year: Harvard Pilgrim Health Care and Maine Community Health Options.
Anthem previously announced that it is exiting Nevada, Ohio, Indiana, Wisconsin and parts of four other states.
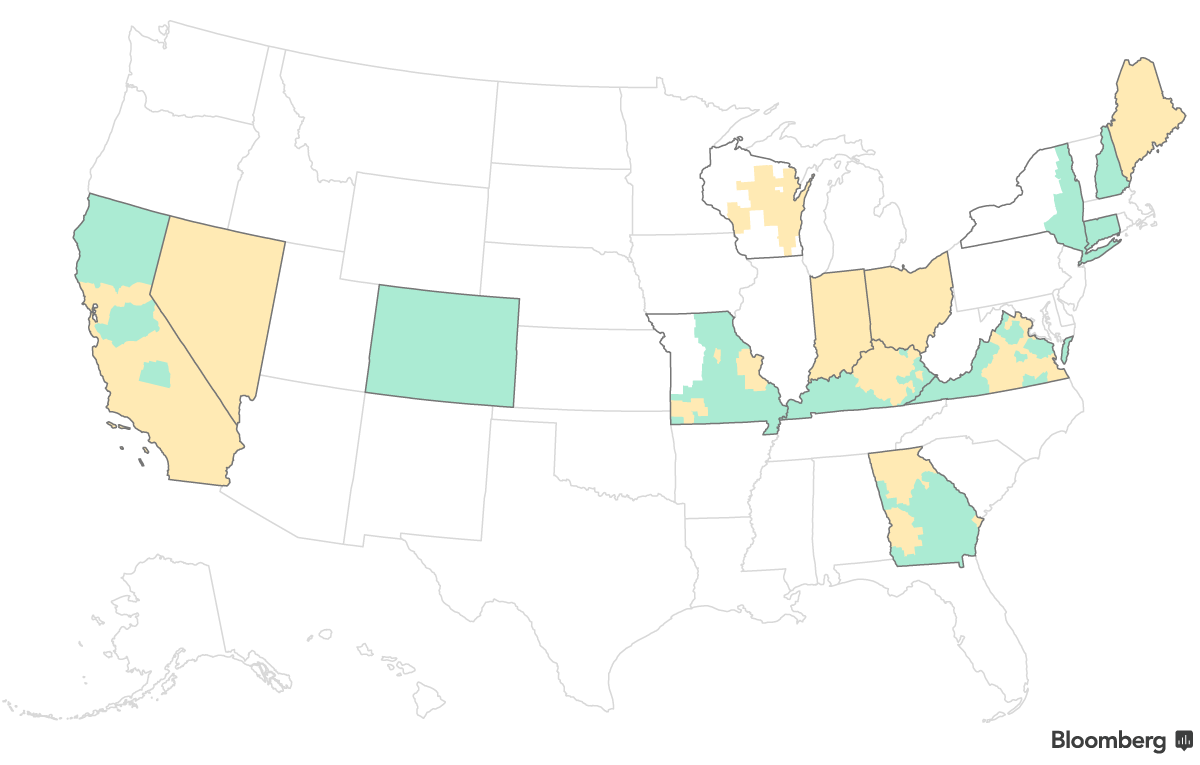
Anthem Reverses Virginia Exit, Fills Remaining Bare Counties
Anthem announced Friday that it will remain in 68 Virginia counties and cities next year, filling all 58 counties that had been at risk of having no insurers next year. The company had announced on August 11 that it would completely exit Virginia’s marketplace, but decided to stay after other company exits had left tens of thousands of Virginia enrollees with no marketplace options. Anthem sold plans in 130 Virginia counties in 2017 under its HealthKeepers brand.
Barring additional exits, all counties nationwide will have marketplace options in 2018.
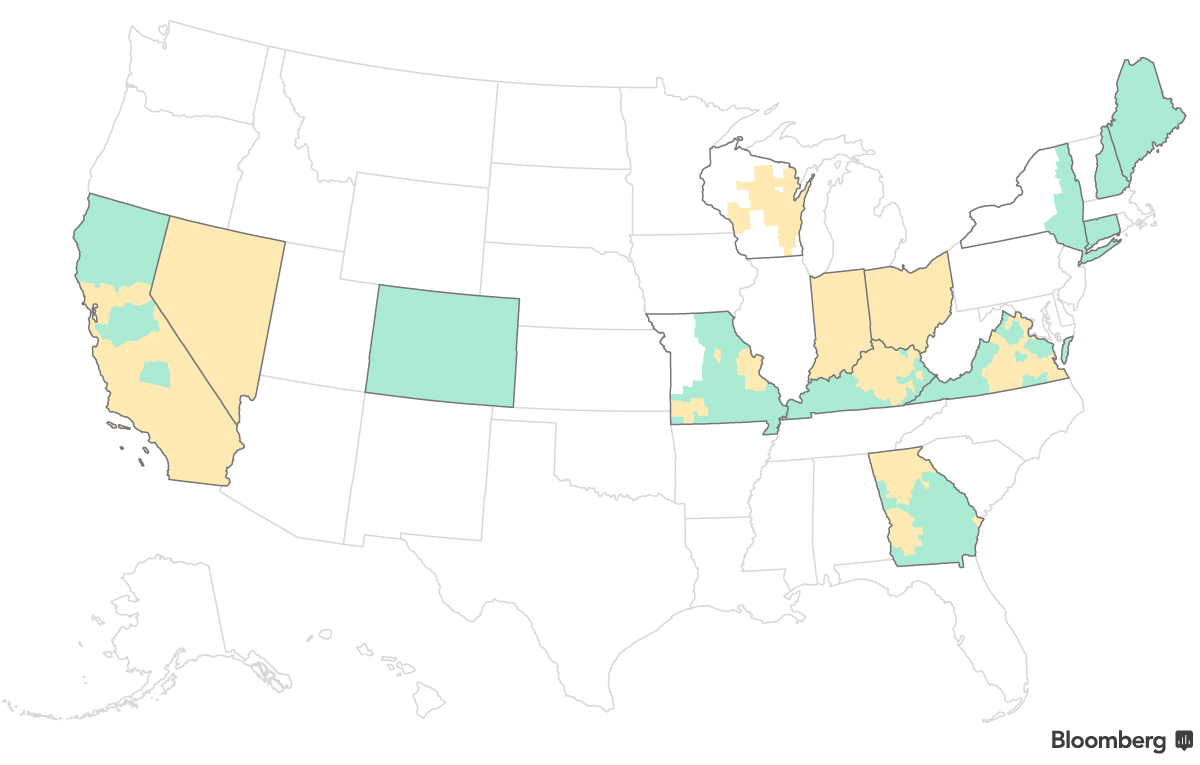
Optima Fills Five Bare Virginia Counties
Optima Health Plan revised its filings this week to sell marketplace plans in six additional Virginia counties, five of which would otherwise have no marketplace insurers next year. Sixteen percent of Virginia enrollees live in the remaining 58 counties that currently have no insurers lined up, but insurers still have time to cover those regions.
Optima’s Reduction of Coverage in Virginia May Leave 63 Counties Bare
Seventy-thousand Obamacare enrollees in Virginia may be without insurance options next year after Optima Health Plan announced Wednesday that it is reducing its presence in the state. Optima, which served in 35 of the state’s counties and county-equivalents in 2017, had planned to cover nearly the entire state next year. Instead, Optima will exit about half of the counties it served in 2017 and enter only the Charlottesville area, Halifax County and Mecklenburg County.
Optima told regulators that it “anticipates a substantial increase in membership due to the recent announcement of market exits by other issuers.” Several carriers including Anthem, Aetna and UnitedHealth have announced plans to exit Virginia entirely next year.
A spokesman for the state’s insurance regulator said that the department “is engaged in serious ongoing discussions with potential carriers to try to fill the gaps.” This year, there were 70,356 Virginians enrolled in the 63 counties where no insurers currently plan to sell plans through the Affordable Care Act’s markets.
Anthem also announced Wednesday that it is exiting the 61 Kentucky counties where CareSource offers plans. Anthem will remain in 59 Kentucky counties that otherwise would not have marketplace options, as it did recently in Missouri and Georgia.
Anthem Scales Back in Missouri, Bright Health Enters Alabama
Anthem is scaling back its Obamacare offerings in Missouri to 68 counties for next year, from 85 this year. The insurer said it’ll remain only in counties where it’s the only option for consumers. That’s similar to the insurer’s retreat from parts of Georgia. Anthem, which offers health plans under the Blue Cross and Blue Shield brand, had previously been an Obamacare stalwart. But it’s retreating from the program this year citing a shrinking market and uncertainty fostered by the Trump administration.
Meanwhile, startup insurer Bright Health is expanding. The company will sell ACA plans in the Birmingham, Alabama-area for 2018, giving individuals in the region a second option. The company sold Obamacare plans in the Denver-Boulder part of Colorado this year, and will again offer plans there.
No Bare Counties: All U.S. Counties to Have Marketplace Options Next Year
Ohio’s Department of Insurance announced Thursday that CareSource will sell marketplace plans next year in the state’s last potentially “bare” county. Paulding County had been at risk of having no marketplace insurers next year after Anthem, its sole insurer this year, exited the state’s marketplace.
Earlier this summer, 19 other counties in Ohio, as well as counties in states including Nevada, Indiana and Missouri, faced the possibility of having no insurer next year. Insurers have since filed to sell plans in all of those areas.
Centene To Cover Nevada’s Bare Counties
Nevada Governor Brian Sandoval announced on Tuesday that Centene will sell marketplace plans next year in 14 of the state’s counties that previously had no insurer lined up. Centene had previously planned to sell only in the state’s most populous areas but will now sell statewide.
Nevada’s rural counties had been at risk of having no insurers next year after Anthem and Prominence HealthFirst chose to exit the state’s marketplace. UnitedHealth will continue to sell plans under its Health Plan of Nevada brand in Clark, Washoe and Nye counties, where 91 percent of Nevada’s enrollees live.
Centene is signficantly expanding its marketplace presence next year in several states. Earlier this summer, the company decided to provide coverage in some Missouri, Ohio and Indiana counties that otherwise would have had no marketplace insurer next year.

Centene Fills Last Bare Indiana County
Centene has revised its Indiana filing to add seven counties next year, including one, Wayne County, that previously had no insurer lined up. The 1,166 marketplace enrollees there were at risk of having no marketplace plans after Anthem and MDWise exited the state.
Under its Ambetter brand, Centene now plans to sell in 49 Indiana counties next year, up from 32 in 2017.
Anthem Exits Virginia Marketplace
Anthem announced on Friday that they won’t sell marketplace plans in Virginia next year. Customers in areas of the state that only had Anthem this year will still have an insurer in 2018, as Optima Health Plan filed for a major expansion next year that includes all of these counties.
Anthem previously announced that it will exit the marketplaces in Nevada, Ohio, Indiana, Wisconsin, most of California and parts of Georgia.

Anthem Exits Nevada, Parts of Georgia
Anthem, one of the largest marketplace insurers in 2017, continues to scale back where they’ll offer plans next year. The Nevada Division of Insurance announced today that Anthem will leave the state entirely after initially planning to remain in three counties.
Anthem is also leaving the 74 Georgia counties that have other marketplace options, while remaining in the 85 mostly rural counties where it is the only insurer. According to Jay Florence, Georgia’s deputy insurance commissioner, the company initially proposed leaving all counties except one. The state’s insurance department said it would respond by banning Anthem from re-entering the market for five years, so the company chose to continue offering plans in some counties.
Customers in the Atlanta metro area, where most Georgia marketplace enrollees live, will still have a choice between two companies next year.

Anthem previously announced that it will exit the marketplaces in Ohio, Indiana, Wisconsin and most of California.
CareSource Revises Indiana Plans to Sell in Three Bare Counties
Three Indiana counties with a combined 2,528 marketplace enrollees are no longer at risk of having no insurer next year. After Anthem and MDWise left the state and CareSource initally planned to drop several counties, Grant, Decatur and Jackson counties were at risk of having no marketplace options. Now, CareSource plans to offer insurance in those three counties next year, based on revised filings submitted by the company in late July.
Molina’s Marketplace Pullback May Extend to More States
Molina announced on Tuesday that it will be exiting the Wisconsin and Utah marketplaces and eliminating about 1,500 jobs after posting large second-quarter losses. The company said it still might exit additional areas and plans to raise rates sharply in its remaining states.
They had previously announced plans to leave several counties in Washington. Molina currently has 950,000 marketplace customers across nine states, according to a spokeswoman.
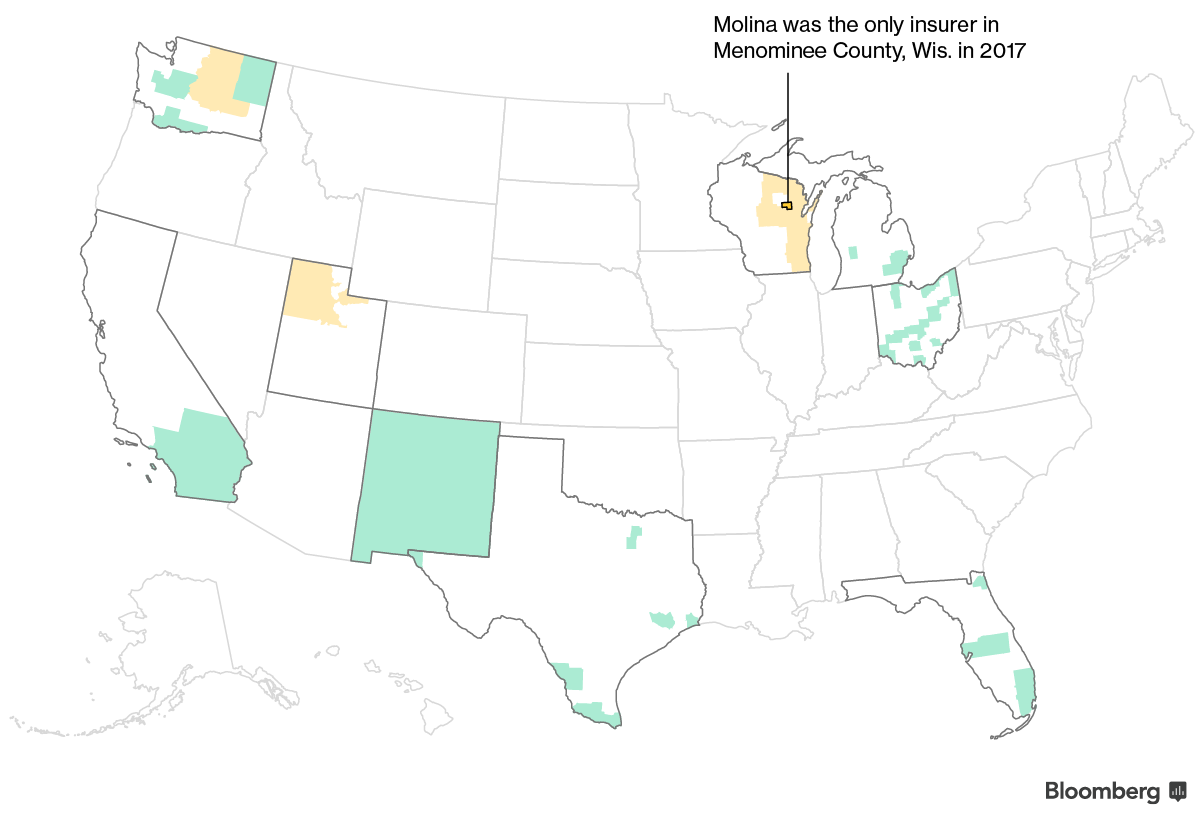
Their exit leaves one Wisconsin county, Menominee, and its 47 enrollees, without marketplace options next year if no other insurer files there. Molina is currently the only insurer planning to sell plans next year in five counties in Ohio and Washington, where a combined 2,121 customers enrolled this year. If Molina leaves those counties, insurance regulators would face a tight scramble to convince other companies to enter before a mid-August deadline.
Molina Exits Wisconsin and Utah
Their exit leaves one Wisconsin county, Menominee, and its 47 enrollees, without marketplace options next year if no other insurer files there. However, full county details are not yet available from every Wisconsin insurer. An official with the Wisconsin Office of the Commissioner of Insurance said that coverage areas are subject to change and that they are working to ensure that all counties are covered.

Molina sold plans in seven Utah counties in 2017, but customers in those counties will still have options. SelectHealth and University of Utah Health Insurance Plans will sell plans statewide next year.
Anthem Exits About Half of California Counties While Centene Expands
California's marketplace announced today that Anthem will be exiting about half of the state's counties, where it serves 153,000 customers, while Centene's Health Net is expanding in the Sacramento area and southern California. Next year, 85 percent of California enrollees will have a choice between three or more companies.
Ohio Finds Insurers to Fill 19 Empty Counties
Ohio has found insurers to offer Obamacare health plans in 19 of 20 counties that had been at risk of having no options for next year, convincing five health insurers to expand in the state. The new expansions will fill gaps left by Anthem and Premier Health Plan’s exits. The state is working to find an insurer for Paulding County, which had 334 enrollees this year.

Competition in Pennsylvania Stays Steady
Pennsylvania released 2018 insurer filings today, and assuming the Affordable Care Act remains law, all of the state’s marketplace companies plan to return next year. As typically happens, a few companies made minor changes in the counties they’ll serve. Competition in the state remains strong—95 percent of Pennsylvania enrollees will have a choice between two or more companies next year.
Medica Expands in Wisconsin, Dakotas Keep Their Companies
Today is the deadline for insurance companies to file their 2018 plans in Wisconsin. One company, Medica, announced today that they’ll offer plans in 21 counties next year, eight more than they offered this year. A spokesperson for the company also confirmed that they’ll continue selling in the same counties in Minnesota, North Dakota, Nebraska and Iowa.
Bloomberg News has also confirmed that coverage options in North Dakota and South Dakota won’t change next year. Spokespeople for Sanford Health Plan and Avera Health Plans in South Dakota confirmed that each will continue to sell marketplace plans statewide. In North Dakota, Sanford and Blue Cross Blue Shield will continue selling statewide while Medica will continue selling in 49 counties there, according to spokespeople for the companies and the North Dakota Insurance Department.
2018 Marketplaces Take Shape
Proposed marketplace offerings for the next year typically fluctuate until states and companies set final plans in the fall. Ongoing efforts to repeal Obamacare are adding even more uncertainty for 2018. In their filings, many companies have also noted that the Trump administration’s non-enforcement of the individual insurance mandate and uncertainty over the continuation of cost-sharing subsidies have caused substantial rate increases for next year. Several companies also wrote in their filings that if cost-sharing subsidies are not funded they will withdraw from the marketplace entirely.
Major Exits and Expansions
A few multistate companies have announced that they won’t be returning next year. Humana is exiting the individual market in the 11 states where it currently sells plans. Aetna is also leaving the few states where it sold marketplace plans in 2017, but will begin selling marketplace plans in parts of Nevada.
Anthem, which sells under the Blue Cross Blue Shield brand, is exiting the marketplace in Ohio, Indiana, Wisconsin and most of Nevada but will continue to sell marketplace plans in several other states.
Still, some companies plan to expand their coverage next year. Centene, which sells under brands including Ambetter, Celtic and Health Net, announced in June that it would sell Affordable Care Act plans in three additional states: Kansas, Missouri and Nevada. The company also said it will expand in six states where it already offers Obamacare plans: Florida, Georgia, Indiana, Ohio, Texas and Washington. Centene will be exiting Massachusetts, however, citing low enrollment.
We don’t yet know where Centene plans to expand in Florida, Texas or Ohio.

Oscar Insurance Corp., which currently sells marketplace plans in parts of New York, California, and Texas, also announced plans to enter several states and expand in California and Texas.
What We’re Watching
As of mid-July, there are about 25,000 people living in counties where no marketplace insurers signed up to sell plans next year. Company decisions are still in flux, and this number will likely change multiple times before open enrollment begins.
Earlier this year, it looked like parts of Tennessee and parts of Missouri could also be so-called “bare” counties, but Blue Cross Blue Shield of Tennessee and Centene, respectively, later filed to sell in those areas. In previous years, every county has had at least one insurance company selling marketplace plans by the time open enrollment began in the fall.
We’re watching Nevada closely. Four companies filed to sell plans this year in Clark, Washoe and Nye counties - where 91% of the state’s enrollees live. No companies filed to sell plans in the other 14 Nevada counties, where about 8,000 people total enrolled in marketplace plans this year. Earlier this summer, the state legislature passed a "Medicaid-for-all" bill that would allow people to buy Medicaid coverage on the state exchange beginning in 2019, but Republican Governor Brian Sandoval vetoed that plan.
There are also 20 counties in Ohio that may have no insurers lined up after Anthem, Humana and Premier Health Plan announced their exits from the state. According to a spokesperson for the Ohio Department of Insurance, no companies have filed to sell in those 20 counties as of July 12, but companies still have time to revise their plans. Ohio will release 2018 filings after final determinations are made in August.