Track the Key Changes in the GOP’s Health Plan
Seven years after the Affordable Care Act was enacted, Republicans are trying to follow through on their promises to get rid of it. While House Republicans passed a repeal bill in May, Republicans in the Senate failed to get their own bill through in July.
Now they're going to try again. A bill by senators Bill Cassidy of Louisiana and Lindsey Graham of South Carolina would shift funds from the federal government to the states, allowing them to choose how to spend health-care dollars. States that expanded Medicaid under the Affordable Care Act would generally lose funds, while states that still have high uninsured rates would generally get additional money. Under Senate rules, they have until September 30 to pass the bill with a simple majority.
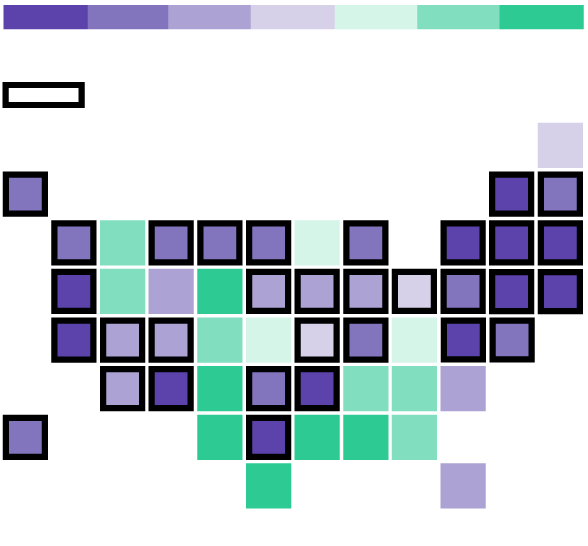
-$1K
-500
-250
-100
0
+100
+250
+500
Expanded Medicaid
ME
AK
VT
NH
WA
ID
MT
RI
ND
MN
WI
MI
NY
MA
OR
UT
WY
DE
SD
IA
IL
OH
PA
NJ
CT
CA
NV
CO
DC
MD
NE
MO
IN
WV
VA
AZ
NM
KS
AR
KY
TN
SC
NC
HI
OK
LA
MS
AL
GA
TX
FL
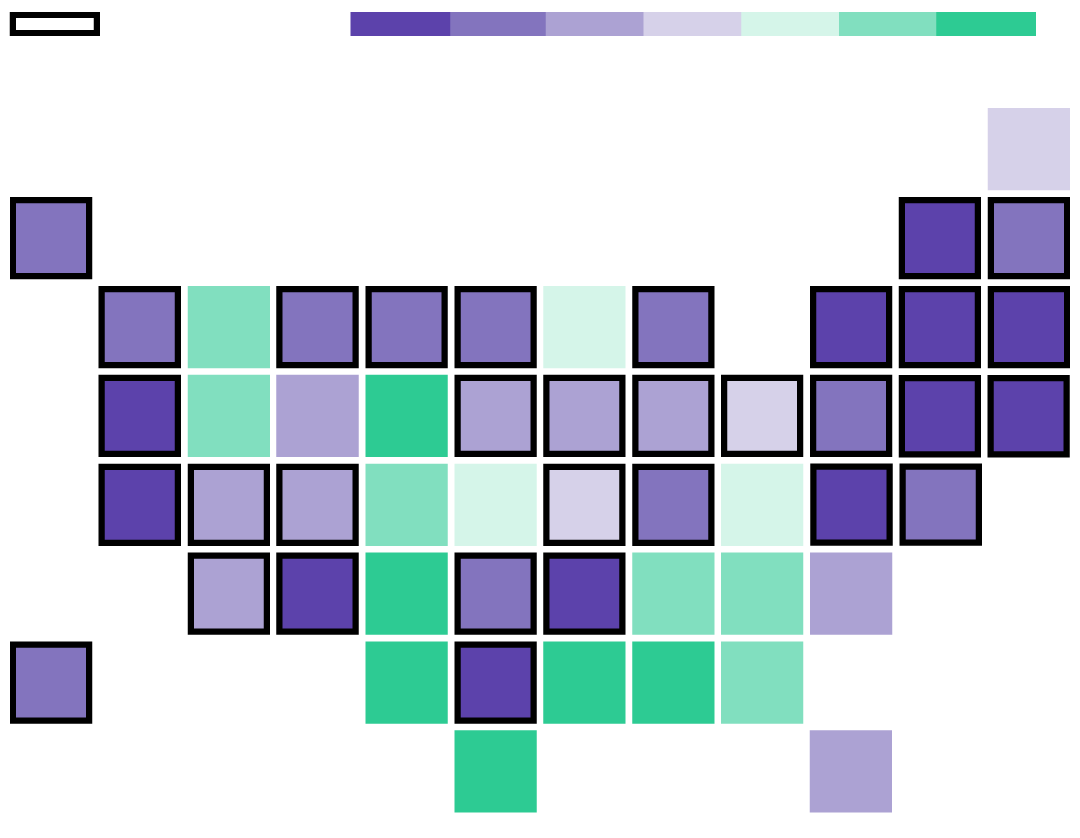
Expanded Medicaid
-$1,000
-500
-250
-100
0
+100
+250
+500
ME
AK
VT
NH
RI
WA
ID
MT
ND
MN
WI
MI
NY
MA
DE
OR
UT
WY
SD
IA
IL
OH
PA
NJ
CT
DC
MD
CA
NV
CO
NE
MO
IN
WV
VA
AZ
NM
KS
AR
KY
TN
SC
NC
HI
OK
LA
MS
AL
GA
TX
FL
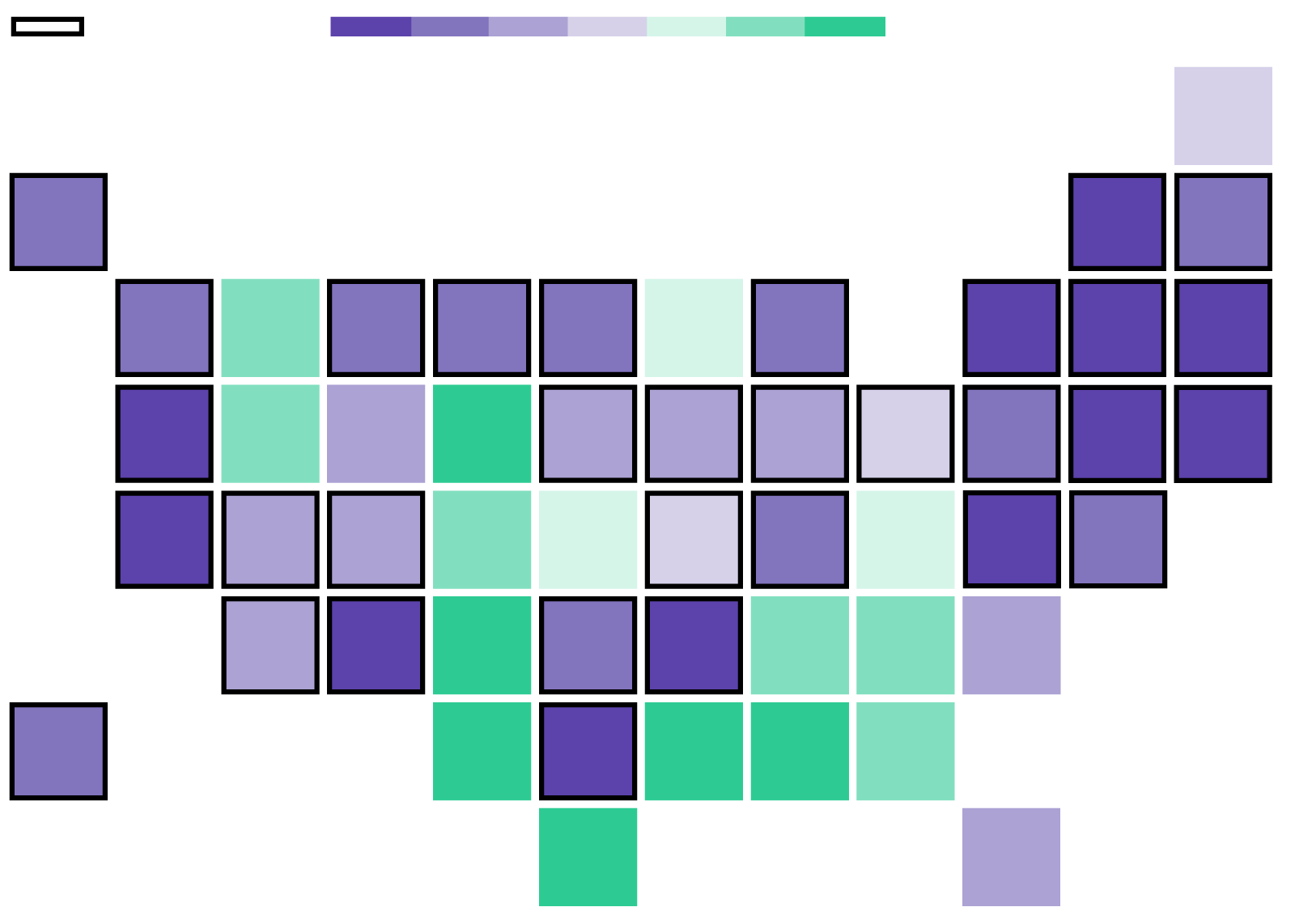
Expanded Medicaid
-$1,000
-500
-250
-100
0
+100
+250
+500
ME
AK
VT
NH
RI
WA
ID
MT
ND
MN
WI
MI
NY
MA
DE
OR
UT
WY
SD
IA
IL
OH
PA
NJ
CT
DC
MD
CA
NV
CO
NE
MO
IN
WV
VA
AZ
NM
KS
AR
KY
TN
SC
NC
HI
OK
LA
MS
AL
GA
TX
FL
If the Senate passes a plan, the House would still need to approve it before the bill reaches President Donald Trump's desk. There probably isn't time for the House and Senate to further negotiate and revise a bill before the Sept. 30 deadline.
Senate bill introduced [June 22] ⟶ Senate vote fails [July 28] ⟶ Passes Senate ⟶ House and Senate negotiate and revise bill ⟶ House and Senate pass final bill ⟶ President signs, becomes law
Includes a new $100 billion fund designed to help states stabilize their individual health insurance markets or help low-income people get health care.
Adds $15 billion to the fund to be used for maternity, newborn, mental health and substance abuse coverage.
Adds $15 billion for the Federal Invisible Risk Sharing Program, designed to help insurers cover the costs of sick and expensive patients.
Adds $8 billion in funding from 2018 through 2023 to help individuals afford higher premiums in states that let insurers charge sick people more.
The Senate bill would include $112 billion in state grant funds, primarily to stabilize state insurance markets and cover expensive patients. It would also allocate $2 billion in 2018 for substance abuse treatment.
The Senate revision would add an additional $70 billion for market stabilization and $45 billion in grants to states toward combating the opioid crisis. A share of the grant funds would be earmarked for states with very high premiums—based on 2017 data from the Centers for Medicare and Medicaid, Alaska is the only state that would qualify.
The Cassidy-Graham plan is built on the idea of sending federal dollars to the states in the form of block grants, giving them broad latitude to use the funds. The total funding in 2020, the first year of the plan, would be $146 billion, less than under Obamacare, according to the Center on Budget and Policy Priorities. The plan evens out how much money the states get, reducing funding to states like California and Louisiana that expanded Medicaid, and benefiting states that didn't, like Texas and Georgia. The plan also provides $25 billion in short-term funding to help stabilize the individual market.
The ACA allowed states to expand Medicaid to individuals making as much as 138 percent of the federal poverty level, with federal funding. The GOP bill winds down Obamacare's Medicaid expansion starting in 2020.
Won't provide extra funding to states that newly expand Medicaid.
Medicaid expansion funding would be phased out between 2021 and 2024.
The expansion would end Dec. 31, 2019. No state can expand if they hadn't done so by Sept. 1, 2017.
Currently, the federal government generally reimburses states for a fixed percentage of Medicaid expenditures, regardless of total spending or number of enrollees. The GOP bill would limit Medicaid reimbursement by a per-enrollee cost, based on 2016 average costs.
Allows states to choose from two formulas for how they get federal Medicaid funding, and boosts the funding for elderly and disabled Medicaid enrollees, relative to the initial bill.
Like the House bill, the Senate bill would allow states to choose between two formulas for federal Medicaid funding. But starting in 2025, the Senate bill would set a lower funding growth rate than the House bill would, meaning states would receive less money. Certain Medicaid enrollees would not be subject to these limits, including people with disabilities and children.
Hospitals in states with high uninsured rates would receive extra funds, changing how “disproportionate-share” payments are calculated. A new program would help states continue to provide some medical services to Medicaid beneficiaries in their homes, rather than moving them to nursing homes. During a state public health emergency, additional spending would not be subject to the new Medicaid caps.
The funds that states received for the Medicaid expansion would be used to help form the basis for the formula that determines their block grants. States can use up to 20 percent of the grants on the traditional Medicaid population. Traditional Medicaid would be limited to a per-enrollee cost.
The ACA introduced subsidies based on income and the cost of health insurance, with some help available to people making up to 400 percent of the poverty level, or about $47,000 for an individual. The House bill would base subsidies mainly on age, phasing out funding beginning at an income of $75,000 for an individual.
The Senate bill would maintain the ACA's subsidies through 2019, but change how subsidies are allocated starting in 2020. The ACA calculates subsidies based on a mid-level coverage plan, while the Senate bill would use a cheaper type of plan. Subsidies would no longer be available to those above 350 percent of the poverty level, or about $42,000 for an individual.
The Affordable Care Act allowed marketplace insurers to sell low-cost catastrophic plans, which have high deductibles and restrict eligibility to young adults and people with financial hardships. The Senate revision would allow anyone to purchase these plans and make them newly eligible for subsidies.
The legislation eliminates the premium subsidies starting Jan. 1, 2020, and uses the funds to help form the basis for the formula that determines states' block grants.
The House bill ends Obamacare's requirement that individuals have health coverage and that most employers offer it. Instead, when people who've gone uninsured decide to buy health insurance, they'll have to pay a 30 percent surcharge on their premiums for one year.
The Senate bill ends Obamacare's requirement that individuals have health coverage and that most employers offer it.
To replace Obamacare's mandate, the Senate bill would impose a six-month waiting period before new insurance goes into effect for anyone who had a break in coverage of at least 63 days in the prior year. The provision takes effect in 2019.
As in previous bills, ends Obamacare's requirement that individuals have health coverage and that most employers offer it. States may use their funding to enter agreements with insurers to encourage people to buy coverage.
The ACA requires health insurance plans to cover 10 broad categories of essential health benefits, as well as to provide preventive services at no cost. The bill initially left the requirement intact, but an amendment that would repeal that requirement was added. Instead, states will define their own list of benefits that are required for plans receiving premium subsidies beginning Jan. 1, 2018.
An amendment was added that would leave essential health benefits intact—reinstating the federal standard. Instead, states could opt out of the requirement and apply for a waiver to define their own list of benefits that are required for plans receiving premium subsidies beginning Jan. 1, 2020.
Adopts changes in House bill.
An amendment would provide insurers broad latitude to sell individual insurance plans that don't comply with Obamacare's mandates. To do so, they'd have to also offer subsidy-eligible Obamacare plans on the marketplaces.
States could choose to obtain waivers to lift the requirement on insurers to cover essential health benefits.
The ACA requires health insurers to sell plans to individuals who are sick with so-called pre-existing conditions and not charge them more than healthy customers. An amendment would allow states to apply for a waiver that would let insurers charge higher premiums to people with pre-existing conditions that had a gap in coverage of at least 63 days in the prior year. To do so, states would have to establish some method (a special “high-risk” insurance pool, or subsidies) to help sick people.
Insurance companies would not be allowed to charge customers with pre-existing conditions more than healthy customers.
States must explain how they will maintain access to adequate and affordable coverage for people with pre-existing conditions.
Obamacare lets health insurers charge their oldest customers no more than three times as much as their youngest ones. The GOP bill introduced widens the ratio to 5 to 1.
Adds a provision that would let the Senate decide whether to increase subsidies that go to older Americans.
Adds a provision that would allow states to apply for a waiver to give insurers permission to charge older customers even more than the 5 to 1 ratio.
Adopts changes in House bill.
States may apply for a waiver to “any provision that restricts the criteria which a health insurance issuer may use to vary premium rates.”
Gives states the option of requiring some Medicaid recipients to work or pursue job training.
Adopts changes in House bill.
As in previous bills, gives states the option of requiring some Medicaid recipients to work or pursue job training.
Ends all federal funding for Planned Parenthood for one year. The bill also prohibits federal funds from going to insurance plans that cover abortions, other than those necessary to save the life of the woman, or in cases of rape or incest.
Adds additional safeguards to prevent government funds from being used for some abortions.
Adopts changes in House bill.
As in previous bills, ends all federal funding for Planned Parenthood for one year. Prohibits federal funds or credits from going to insurance plans that cover abortions, other than those necessary to save the life of the woman, or in cases of rape or incest.
Repeals a 0.9 percent Medicare payroll surtax and a 3.8 percent investment-income tax on wealthy individuals that were introduced in the ACA, effective 2018.
Ends the taxes in 2017, rather than 2018.
Postpones repeal of the additional Medicare tax to 2023.
Adopts the tax repeals in House bill.
Keeps both the 0.9 percent Medicare payroll surtax and the 3.8 percent investment-income tax on wealthy individuals. Allows the purchase of health insurance with funds from a health savings account, which provides tax advantages.
Keeps both the 0.9 percent Medicare payroll surtax and the 3.8 percent investment-income tax on wealthy individuals.
Repeals ACA taxes imposed on health insurers, pharmaceutical companies, medical-device companies and tanning salons, effective 2018.
Ends the taxes in 2017, rather than 2018.
Repeals most taxes immediately. A tax on providers would be phased out in 2025.
Repeals the tax on medical devices in 2018, but leaves other industry levies in place.
Obamacare imposes a tax on very generous health insurance benefits, which was delayed to 2020. The bill introduced further pushes the tax back to 2025.
Delays the tax to 2026.
Adopts changes in House bill.
Leaves an Obamacare tax on very generous health insurance benefits in place.
The ACA requires health insurers to allow children to remain on their parents' plans, up to age 26.