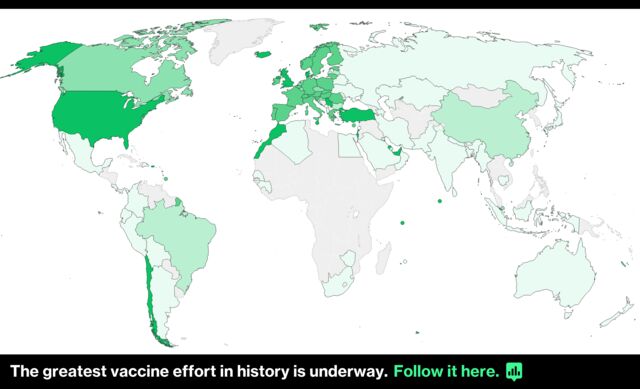
How the U.S. Is Vaccinating Its Way Out of the Pandemic
After a year of anxiety and isolation, millions of Americans a day are getting immunized against Covid-19, and starting to get their lives back.
On Dec. 14, 2020 a milestone was reached in the U.S.
The nation’s first Covid-19 vaccine started to arrive at hospitals across the country, nine months after the coronavirus shuttered the U.S. economy, killed hundreds of thousands and wreaked havoc on every aspect of American life. That day reflected both a landmark scientific achievement and a logistical triumph.
Cameras captured Sandra Lindsay, a critical care nurse, receiving a shot of Pfizer Inc. and BioNTech SE’s vaccine in New York. Lindsay became the first known person to get the vaccine in the U.S. following regulatory clearance.
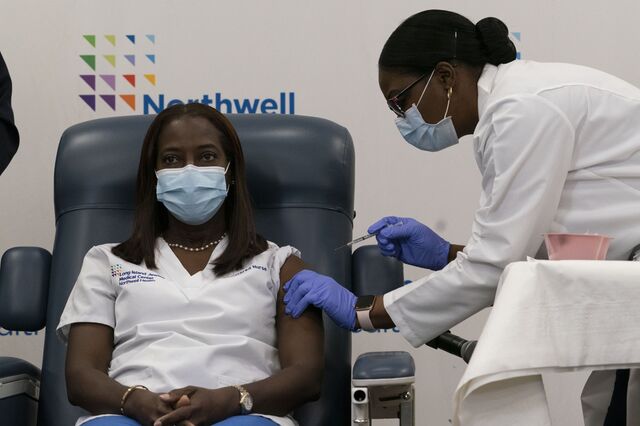
“I just kept saying, I cannot believe, the moment I’ve been waiting for, it’s finally here,” said Lindsay, director of nursing at Northwell Health’s Long Island Jewish Medical Center. “This is what we need to stop all of this harm and suffering.”
Vaccines promise to end a pandemic that has already claimed about 550,000 lives in the U.S. alone—if they reach enough people. At least 70% of the population needs an inoculation to reach herd immunity. Immunizing the country’s 255 million adults will require almost twice as many shots since two of the three currently available vaccines use two doses.
Months before the first shots were administered, the Centers for Disease Control and Prevention and the Department of Defense coordinated with state leaders to map out where they would send those shipments. Fresh deliveries of three vaccines from Pfizer-BioNTech, Moderna Inc. and Johnson & Johnson are now sent weekly. 145.8 million doses have been administered. 28.6% of the population has received at least one shot.
The success has not come without strife. People have spent hours searching fragile websites for an elusive appointment. Winter weather delayed deliveries. Administration of vaccines has not been equitable, with minority communities falling behind in immunization.
Despite the challenges, the work is paying off.
“It feels like a more optimistic time,” said Joseph Kanter, a Louisiana Department of Health official. Kanter spoke on March 12, the week Louisiana commemorated the one-year anniversary of the first case in the state, the first time the number of shots administered exceeded the number of new cases and the fewest nursing home cases recorded since the state started counting.

Michael and Phyllis Addison, pastors in Randallstown, Maryland
Michael and Phyllis Addison started New Life Restoration Ministries last spring. They host services via Zoom, usually drawing a congregation of about 45 from near and far. They started using their sermons to educate parishioners about the need to get vaccinated against Covid-19.
Yet they struggled to find shots for themselves. Michael Addison is 70 and Phyllis Addison is 68. First, they needed to figure out how to register. Then they heard signing up multiple times would push them to the back of the queue.
“It’s like we’re running into one thing and then another,” Phyllis Addison said in mid-February of the issues the Black couple and others have experienced getting vaccinated.
It took them a month before they snagged appointments. A parishioner’s daughter found them an appointment at M&T Bank Stadium in Baltimore. Yet they heard horror stories of hours-long lines and switched their appointment when they received an email to register at LifeBridge Health's Northwest Hospital, a five-minute drive from their home.
“At one point everything was closed down, you couldn’t get an appointment,” Phyllis Addison said. “And then all of the sudden because of the availability of the shots, everything opened up.”
The Addisons got their first Pfizer shots on March 23. It took about an hour, they said by telephone that evening. Michael Addison was nervous because he doesn’t like needles. Phyllis Addison worried whether she would have side effects. Staff at the hospital encouraged them to relax, walked them through the process and eased their fears.
The pastors planned to share their experience with their congregation during Sunday services and further encourage others to get vaccinated. Services will stay virtual for the time being, though they have started looking at buildings to host in-person worship.
Michael Addison relates the vaccine to salvation: “It’s best to have something and not need it than to need something and don’t have it.” “That’s it,” Phyllis Addison said. “That’s the reality of it.”

Ann Hilton Fisher, retired lawyer in Marquette, Michigan
Ann Hilton Fisher, 72, hadn't been able to enter her 96-year-old mother's room in assisted living since March 2020. She last saw her mother in-person during an outdoor visit in October, before winter arrived in Northern Michigan.
“You’d see her on Zoom and you’d think: How is she really? Can I tell?” Hilton Fisher said.
Hilton Fisher was designated an essential caregiver who could help her mother eat twice a day since the arthritis in her fingers worsened, preventing her from feeding herself. That meant she could be vaccinated along with residents and staff on Jan. 19.
“I didn’t see my mother in the vaccination room,” Hilton Fisher said. “I asked if I could swing by and just, you know, wave to my mother. And they said yes. And so that was the first time I had seen her in her room since last March.”
She now sees her mother twice a day—every day.
“It’s just like this huge load is lifted,” she said. “Part of that is the vaccination, but more of that is being able to be with her.”
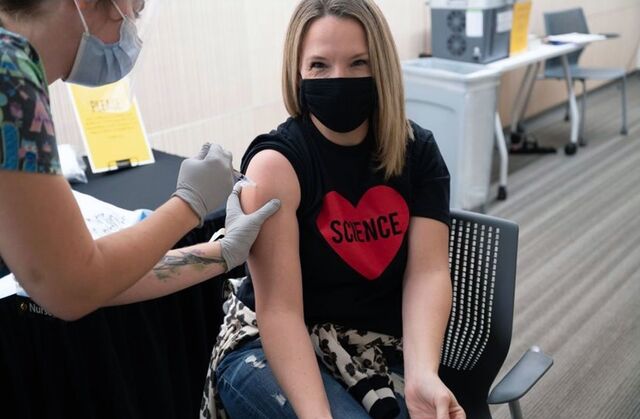
Allison Wynes, 40, nurse practitioner in the medical ICU at University of Iowa Health Care
Allison Wynes, a nurse practitioner in the ICU at the University of Iowa Health Care system, was among the first Americans to become vaccinated, shortly after Pfizer was authorized. She got a shot in front of news cameras the morning of Dec. 14.
“I was just floating on air. And then that feeling was shortly replaced with some guilt and some concern for others who needed to get vaccinated. Guilt for my friends who were working in the ICU with me as providers and weren’t on the list yet.”
“The person sitting directly next to me working in the surge unit hadn’t gotten theirs yet. And I just, you know, you kind of feel bad and I feel a mix of joy and hope, but also like: Oh gosh, this is meaningless unless everyone else gets vaccinated too.”
Yet the vaccines didn’t change the precautions taken in the hospital.
“You go back to work, you put your mask on and put your face shield on. You put your gown on, you put your gloves on and you keep taking care of your patients.”
Pictured: Michael and Phyllis Addison leave the LifeBridge Health vaccine clinic in Randallstown, Maryland, after receiving their Covid-19 vaccine on March 23. Photographer: Rosem Morton/Bloomberg
Pictured: Ann Hilton Fisher embraces her mother once they've both been vaccinated. Courtesy of Ann Hilton Fisher
Pictured: Allison Wynes receives the second dose of the Covid-19 vaccine on Jan. 5. Courtesy of Allison Wynes
Sound is off
In the Room in Vaccine Decision-Making
Paul Mango, former deputy chief of staff of policy at HHS
Paul Mango was the deputy chief of staff for policy at the Department of Health and Human Services during Donald Trump’s presidency. The first meeting he attended about Covid-19 vaccines was in late March 2020.
Remarkably, less than nine months later, on the afternoon of Dec. 10 he watched from the office of Chief Scientific Adviser Moncef Slaoui as advisers to the FDA voted to recommend the Pfizer-BioNTech vaccine. The scientific challenge then yielded to the logistical one. From the operations center on the second floor of HHS headquarters, Mango watched the shots roll out.

“We could track every dose exactly where it was: It was leaving the factory, it was on a truck. Every two seconds we got a satellite message of where each box of vaccines was: on a truck, on a plane. It’s landed, it’s been delivered, it’s been signed for.”
The initial distribution coincided with the holiday season. “Every one of us worked every minute of the holiday,” Mango said. Little distracted the group, which spanned hundreds of employees across HHS and other agencies. The HHS building is adjacent to the Capitol, and Mango worked through the riot at the Capitol on Jan. 6, not knowing the extent of what transpired. “I remember (HHS Secretary Alex Azar) coming into my office saying: Get out of here.” He stayed.
In late December and early January, dashboards showed states had used less than half of their doses. Mango realized there was a lag in reporting. In January officials widened eligibility criteria and sent doses to pharmacies to speed things up.
“We were watching every day the number of reported vaccinations, and it was skyrocketing. It was going up by hundreds of thousands a day,” he said. On the day of President Biden’s inauguration, more than 1.5 million doses were administered. “We were kicked out on the 20th at noon,” Mango said, “and we felt it was a very strong finish.”
Keeping the Vaccines at the Right Temperature
Molly Howell, Immunization Program Manager in North Dakota
North Dakota had been planning for the possibility of Covid-19 vaccines since last May. The state equipped its warehouse with ultra-cold freezers and a dry ice machine so it could receive Pfizer’s vaccine and disperse the vials across the rural state. Shipments started arriving the week of Dec. 14.

“It kind of jump-started us again, you know?” said Molly Howell, North Dakota’s immunization program manager. “There was some frustration. We were just coming off of a wave of cases and hospitalizations and deaths that we had had in November. And so I think the vaccine coming out just gave hope and really got people excited again about what they were going to be able to do, which is prevent future hospitalizations and deaths due to Covid-19.”
North Dakota led the nation in how quickly it used its supply. The state broke up 975-dose Pfizer shipments and even the 100-dose Moderna packages into smaller amounts to send across the state.
“We really emphasized that providers should give doses the week that they received them,” Howell said. “And that we didn’t want any doses sitting in the refrigerator or the freezer.”
Soldiers Getting Shots in Arms
Captain Regan Keenan, officer in charge of the Rhode Island Army National Guard’s Sockanosset Point of Dispensing, The “Sock”
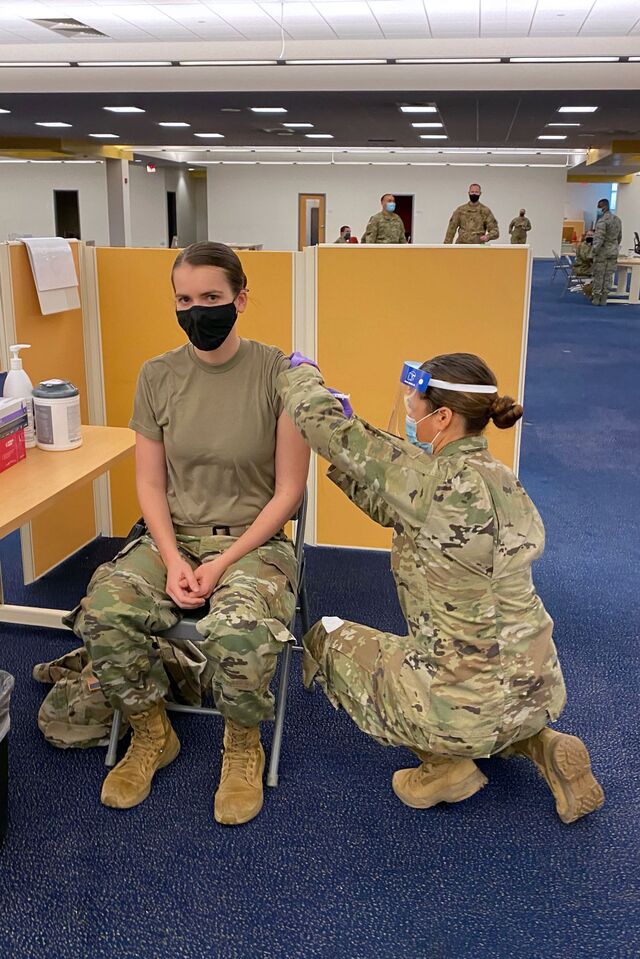
The National Guard was called into vaccination duty in Rhode Island in late December. They used those earliest days at the Cranston clinic to immunize each other and perfect their procedures before they welcomed civilians in mid-January.
“For us, we have check-in stations that are in-line with the vaccinators and we were able to fine-tune the ratio of the right number of check-in stations for vaccinators,” said Captain Regan Keenan from the Rhode Island National Guard, who oversees the Sockanosset Cross Road clinic. “Since we wanted to be able to do as many as we could in an hour, we didn’t want anybody sitting and not doing anything because the station before or behind them was overwhelmed.”
The team initially expected they could vaccinate 100 people an hour. The clinic can now comfortably immunize 350-450 people an hour.
“In the beginning it was a lot more every day having to solve problems and being concerned about new processes and stuff on the floor,” Keenan said. “At this point, we’re really getting into that steady state.”
“The Sock,” as the Guard calls the clinic because it’s located on Sockanosset Cross Road, now gives Pfizer, Moderna and Johnson & Johnson shots.
“Logistically, it’s crazy,” Keenan said. “It’s very, very fast paced.”
“There are a lot of service members walking around the observation area when if they see people who are nervous, they take the time to ask how they’re doing and kind of help talk them through that 15 minutes,” Keenan said. “At the end, there are people who come up and say: thank you. I was very, very nervous, but you guys kind of helped me through it.”
Kristi Larson, operations supervisor at McKesson distribution facility in Kentucky
When the first batch of Johnson & Johnson vaccine was packed at the McKesson facility in Kentucky on March 1, its journey into the box that vaccinators would eventually open had been rehearsed for weeks. Station to station, and really, hand to hand, the process was overseen by Kristi Larson, an operations supervisor at the facility. Her team started preparing when it looked as though the Johnson & Johnson authorization was imminent.
“It was probably three weeks ago, tops, that we had to plan everything, to get everything set up. Each day was filled with so many things that we needed to accomplish, needed to fix, needed to change.”
Larson and her team did dry runs to prepare. They used Irish Spring bar soap to practice handling the vial packs. When the vaccine arrived at the facility on Thursday, Feb. 25, Larson gathered her team around.
“I got them in a group and I said: Alright, we’re gonna go into the vial box real quick, ‘cause I got something fun to show you. I was holding up the first vaccine for them, and then I said, take a look at the vaccine compared to what we were practicing with the soap. It was very similar, but to actually have them see the vaccine firsthand, all of these times and days training, they finally got to see and hold in their hands the vaccine that they were going to be helping distribute.
“There was a quiet moment. Like, this is really happening, all this planning, all of this time we’ve been practicing.”
After the first set of boxes was packed, she personally walked one down to UPS as the team watched and clapped.

Matt Knowlton, United Parcel Service Inc. driver near Providence, Rhode Island
Matt Knowlton’s manager called him over on the morning of Dec. 14 to tell him he’d be taking a box of Pfizer vaccines from the United Parcel Services Inc. hub near Providence, Rhode Island, to Newport Hospital.
“It was kind of a big deal because it was one of the first ones to come through,” Knowlton said. “You felt like you were driving around something important.”
Knowlton would be one of the first people in the U.S. to transport Covid-19 vaccines. Knowlton delivers vaccines almost every day, to places like CVS Health Corp. pharmacies. But he hasn’t yet been eligible for vaccination.
“It’s ironic that we deliver it but don’t get it,” Knowlton said. “As soon as it’s available, I’ll go get it.”
Pictured: Kristi Larson walks a box of J&J vaccine on the first day of deployment at the McKesson facility in Kentucky. Courtesy of McKesson
Pictured: Knowlton loads his first batch of vaccines for delivery at the UPS hub in Providence, Rhode Island. Courtesy of Matt Knowlton
Sound is off
Dispensing Vaccine Information
Joe Smyser, CEO of The Public Good Projects
Smyser runs Project VCTR (Vaccine Communication Tracking & Response), which helps health officials respond to online conversations and misinformation about vaccines. The project pre-dated Covid, yet the pandemic accelerated online chatter.
“We still see a whole hell of a lot of vaccine misinformation and disinformation. And there are a lot of nefarious actors there, mostly domestic, but some international. But we also more than that see just earnest information-seeking.”
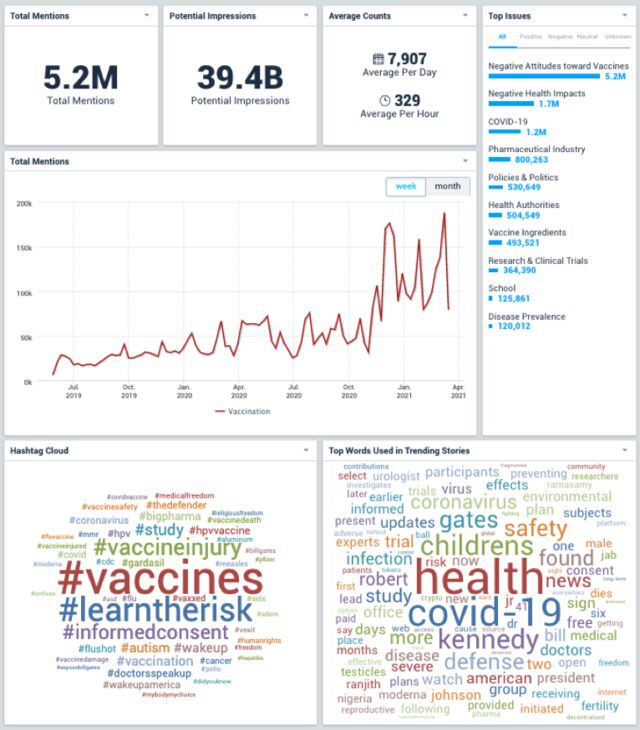
“The intense interest from just about everybody in: how are vaccines made? How do we know that they’re safe? What’s in this vaccine? Let’s talk about the equity of vaccine distribution. All of these topics have never been of interest at the scale that they are now. And there weren’t ready-made answers to the questions.”
For all the misinformation, Smyser also has seen progress as the story of people getting vaccinated is increasingly told online.
“I think it is having a huge impact. I don’t think it’s at the scale that it needs to be, that needs to be happening, especially in communities of color.”
Getting People Comfortable
Judith Shlay, 63, associate director of Denver Public Health
Judith C. Shlay, the 63-year-old associate director of Denver Public Health, saw disparities emerge early in who wanted to be vaccinated once shots became available to anyone 70 and older.
“People who were more savvy in how to use the Internet, information systems, had the ability or had family who could support them—they got registered much faster than people who maybe didn’t speak the language, didn’t know about those things.”
In Denver, officials focused on bringing vaccines directly to communities where vulnerable people lived. Shlay’s name is on the order form for thousands of them.
Denver's Vaccine Disparities
Black and Latino residents suffered a disproportionate share of Covid-19 deaths but have been vaccinated at lower rates than other groups
Source: Denver Public Health
“I would have people come up to me over and over and over and thank me, and I didn’t even know who they were. I mean, in the hospital system, ‘thank you for getting me vaccinated,’ and I didn’t do it, but I’ve ordered probably 60, 65,000 doses of vaccine for people, maybe even more. That’s a lot of vaccine for an agency and for a city.”
“I saw people crying. I saw people just hugging, even though they weren’t supposed to, they were so overjoyed with emotion.”
“For me, it’s just the ability to bring back our society to the way we want it to be again.”
Handling Doses
Lisa Macon Harrison, Director of Granville-Vance Public Health in North Carolina
The early days of the vaccination campaign were spent perfecting processes, especially how to handle leftover vaccines, says Lisa Macon Harrison, who leads Granville-Vance Public Health in North Carolina. Harrison’s staff exchanged notes with pharmacies and hospitals in the area.
“Nobody wants to waste a single dose of this valuable vaccine, so what some of those early conversations were about were really sharing that commitment to each other. Like if I have three doses left at the end of a vaccine clinic and you have a clinic going on that day, too, I’m going to call and tell you I’m bringing you these three vaccines so that you can give it to the people you have and you don’t have to open another vial,” Harrison said.
Granville-Vance Public Health has administered 21,889 vaccines across the health district, including 14,362 first doses and 7,527 second doses, as of Friday, March 26.
“It’s very intense,” Harrison said. “Every day is a new adventure. It’s a very important adventure to get right.”

Jeremy Cauwels, Chief Physician for Sanford Health in Sioux Falls, South Dakota
You could feel the change at Sanford Health when the vaccines arrived. Its 46 hospitals in the Dakotas and Minnesota were ravaged from battling a deadly fall surge.
“I didn’t know you could ever have something feel like hope before, but I think that’s honestly what it felt like,” said Jeremy Cauwels, Sanford’s chief physician. “It was palpable in the room that the vaccinations were going to get us to lower numbers in our hospitals, less stress on our doctors and nurses and all of our health care staff.”
How willing employees are to get vaccinated generally depends on their level of medical training, Cauwels said. More than 85% of the system’s doctors and about 80% of advanced practice providers are immunized. About 65% to 70% of nurses have received the shots and about 35% to 40% of long-term care workers have received them.
“Social media has driven a lot of doubt, as well as reporting on various different things that quite honestly used to happen in a lab with a couple of PhDs and a couple of doctors discussing things around the table,” Cauwels said. “They’re now getting discussed at a national level on the news, and I hate to say it, but those things can sow the seed of doubt into patients that otherwise would have been very accepting of a vaccine.”
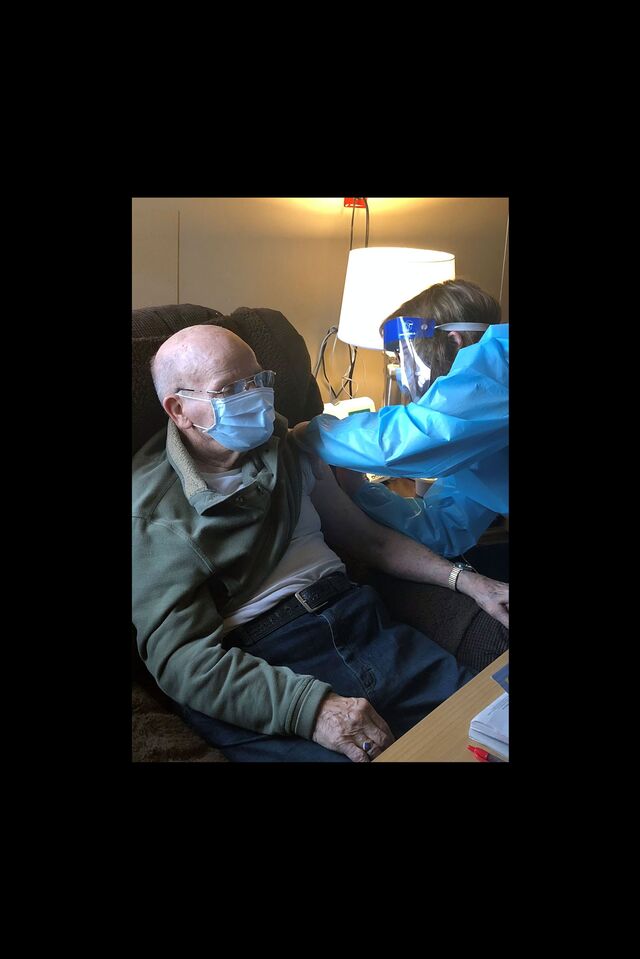
Sondra Norder, Chief Executive Officer of St. Paul Elder Services in Kaukauna, Wisconsin
Sondra Norder spends her days confronting the coronavirus firsthand. She’s the chief executive officer of St. Paul Elder Services in Wisconsin. More than three-quarters of residents at the main campus of the 120-person nursing home tested positive for the virus, and 26 of them died.
“I got to sit with some other staff who were getting vaccinated at the same time as I did. It was like a weight was lifted off of our shoulders in that moment. There were definitely more than a few tears for sure,” Norder said. “I got pretty choked up. It was like a weight lifted off of my shoulders, really the weight of the world. It finally felt like, OK, we’re really getting there. And I think we’ve all been so exhausted that it doesn’t take that much to make us emotional at this point.”

Adrienne Stewart in the Bronx, New York
Adrienne Stewart and her partner Dawn got Johnson & Johnson’s vaccine at Yankee Stadium one night in March around 10 p.m., the earliest appointment they could get that evening.
“Oh my god, I was scared,” Stewart said. “I don’t like needles. And second of all, we don’t know what this is. You know what I’m saying? So I was really scared because I have underlying health issues and I was scared I was going to have a reaction, so a lot of things are going through my mind. But at the end of the day, it had to be done.”
The past year has been marked by constant fear. Stewart, 50, has a slew of health issues, including diabetes, high-blood pressure and COPD, that put her at increased risk of severe illness if she contracted the virus. The couple estimates they didn’t leave their home from March until July.
“We gotta do what we gotta do to keep everybody safe,” Stewart said. “We lost a lot of people, so that played a part.”
When asked how many, she said, “Oh my God, we lost a lot. Maybe about 10,” family and friends. Stewart already knows many people who have been vaccinated.
“We’re going to try to get more to get out here so we can get back to normal,” she said.
Pictured: Katherine Porter, a retired Sanford Health nurse, speaks to the media after receiving her first dose of the Covid-19 vaccine in Sioux Falls, South Dakota in January. Courtesy of Sanford Health
Pictured: A St. Paul Elder Services nursing home resident receives the Covid-19 vaccine. Courtesy of St. Paul Elder Services
Pictured: Stewart's selfie, post-vaccination at Yankee Stadium in the Bronx. Courtesy of Adrienne Stewart
Sound is off
Finding Appointments for Friends
Karen Pelton and Mary Hause, Tacoma, Washington
Karen Pelton, 72, and Mary Hause, 69, this winter became adept at scouring websites to find vaccine appointments for a group of high school friends that reconnected over Zoom during the pandemic.
“As soon as it came up online and as soon as I filled out the information slot, it was gone,” Pelton said of finding an appointment for her husband in late January. “I picked another time, two or three times past the first one. I got him an appointment. I immediately hung up and called my girlfriend. She went in right away and was able to get an appointment. That left us with two people who hadn’t gotten appointments. Two were on a list and I kept trying and two days after that I was able to get one more appointment for one of the guys. It seems like I’ve been trying all different hours.”
The phone tree that started in January eventually helped their entire Zoom group find shots, with some stumbles along the way.
“One friend landed a vaccine for her husband on the Albertsons site,” Hause said. “She said: Get on right away. Then I called Brad. By the time he got on they disappeared in less than a minute.”

Dr. Loretta Christensen, Medical Director for the Navajo Nation, Indian Health Service
Three months into the vaccination campaign in the Navajo Nation, about 70% of the area’s user population—people who have visited a health care facility in the last three years—has received at least one dose of the vaccine.
It’s no small feat in the nation’s largest Indian reservation stretching 27,000 square miles across parts of Arizona, New Mexico and Utah. The region has experienced two devastating Covid-19 surges, at times posting the highest per-capita infection rate in the U.S.
“To have this very tangible way of fighting Covid has been a gift to us here on Navajo,” said Loretta Christensen, chief medical officer of the Navajo Area Health Service.
Christensen pins the success of the campaign to unified messaging with Jonathan Nez, the president of the Navajo Nation, using everything from bilingual radio shows to Facebook Live. That’s accompanied by a coordinated, data-driven effort that has delivered vaccines with and without appointments.
“You do have to have four-wheel capability to get to some of these homes,” Christensen said. “We have a community called Hard Rock. There’s no direct way to get there, and you have to go around the mountain. It’s hard for those people to make that trip, so we sent a strike team.”
They also have relied on the local expertise of community health workers. “They know all of the patients in their areas,” she said. “They can tell you where the houses are, they tell you who lives there. They’ve just been invaluable in us getting out to those communities.”
Pictured: Volunteers separate the Covid-19 vaccine into individual doses at the University of New Mexico's Gallup campus, which hosts Covid-19 vaccinations through the Navajo Area Indian Health Service, on Mar. 23. Photographer: Cate Dingley/Bloomberg
Sound is off
—With Thomas Black
(Updates Jeremy Cauwels title in 71st paragraph.)